Roles of lysosomal small-molecule transporters in metabolism and signaling
Small-molecule transporters of the lysosomal membrane export lysosomal catabolites for reuse in cell metabolism.
These transporters often show substrate promiscuity and, conversely, a given metabolite is often exported through distinct transport routes and sometimes in different states (e.g., single amino acids versus dipeptides).
Some lysosomal transporters import metabolites into the lumen. The combination of importers and exporters can create small-molecule shuttles across the lysosomal membrane, which regulate the lumen state.
Some lysosomal transporters participate in intracellular signaling cascades. sciencenewshighlights ScienceMission https://www.cell.com/trends/cell-biology/fulltext/S0962-8924(25)00222-3 https://sciencemission.com/lysosomal-small-molecule-transporters
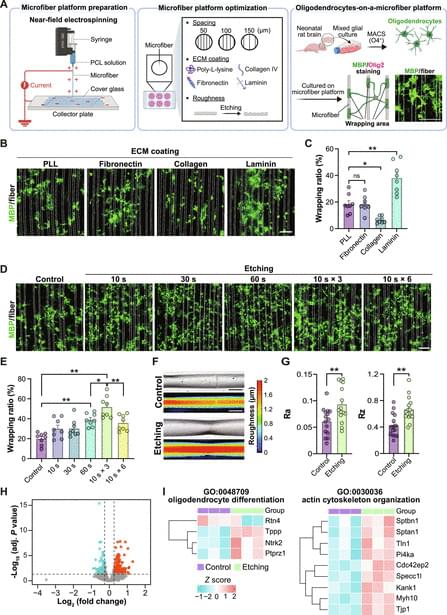
Remyelination requires the precise wrapping of axons by oligodendrocyte processes, a critical step for restoring neural circuit function. However, a lack of quantitative systems that recapitulate axonal geometry and chemistry has limited mechanistic and pharmacological insights into myelin wrapping. Here, we present a bioengineered microfiber platform that mimics neurite architecture and surface chemistry, enabling high-content quantification of oligodendrocyte wrapping. Through compound screening, we identified dimemorfan, a clinically used sigma-1 receptor agonist, as a potent enhancer of myelin wrapping. Dimemorfan treatment accelerated remyelination and functional recovery in demyelinated mice and promoted myelin wrapping by human induced pluripotent stem cell (iPSC)-derived oligodendrocytes.