Researchers with the University of Cincinnati and Johns Hopkins Medicine developed a potential treatment for brain cancer that uses nanofibers embedded with a combination of drugs that work in concert to target tumors. The drugs proved more effective in combination than when administered alone and can provide both immediate and long-lasting doses to kill cancer cells.
“In our study, a three-drug combination showed strong synergistic effects across multiple glioblastoma models and significantly improved survival in animal studies,” said Daewoo Han, an assistant professor in UC’s College of Engineering and Applied Science and lead author of the paper published in ACS Biomaterials Science & Engineering.
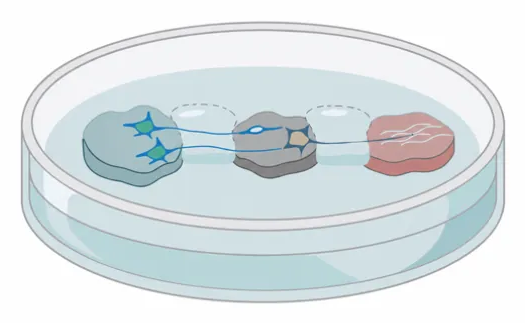
Han and Distinguished Research Professor Andrew Steckl incorporated the drugs into electrospun fiber membranes, creating a nanofiber drug delivery system. Steckl’s NanoLab at the University of Cincinnati is a leading developer of this technology that uses an electric field to create a multilayered fiber mesh for drug delivery, among other uses. “This combination is pretty powerful,” Steckl said.