Scientists are rethinking how to treat a widespread genetic cholesterol disorder by targeting particle production instead of removal.
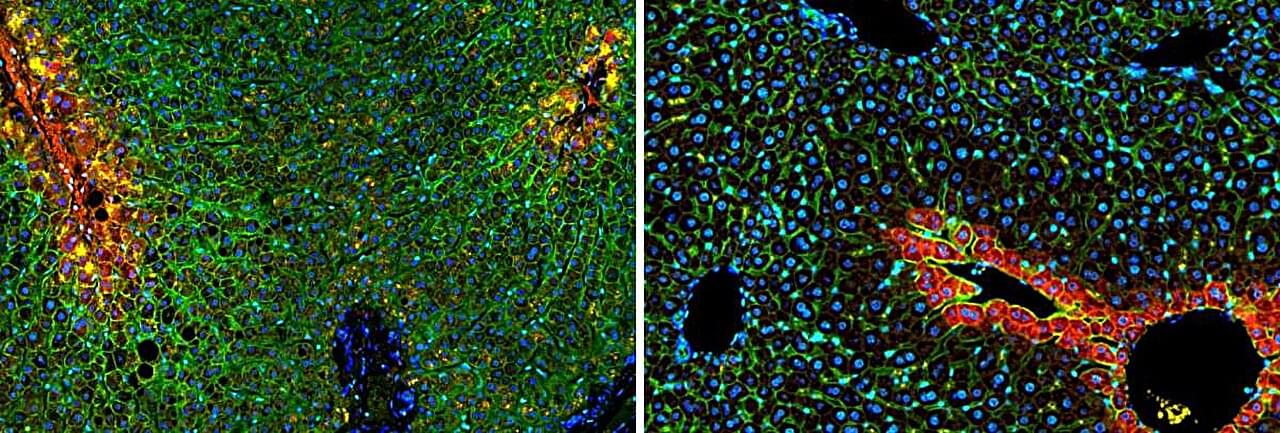
Familial hypercholesterolemia (FH) disrupts one of the body’s most important cleanup systems. Normally, low-density lipoprotein (LDL), often called “bad” cholesterol, is removed from the bloodstream by LDL receptors (LDLR) in the liver. These receptors act like docking stations, pulling cholesterol into cells where it can be broken down. In people with FH, mutations in the LDLR gene weaken or disable this process.
As a result, cholesterol builds up in the blood for decades, often without obvious symptoms until it leads to heart attacks or other cardiovascular problems. About 1 in 200 adults carries this genetic change, making it one of the most common inherited disorders worldwide.