When patients undergo general anesthesia, doctors can choose among several drugs. Although each of these drugs acts on neurons in different ways, they all lead to the same result: a disruption of the brain’s balance between stability and excitability, according to a new MIT study.
This disruption causes neural activity to become increasingly unstable, until the brain loses consciousness, the researchers found. The discovery of this common mechanism could make it easier to develop new technologies for monitoring patients while they are undergoing anesthesia.
“What’s exciting about that is the possibility of a universal anesthesia-delivery system that can measure this one signal and tell how unconscious you are, regardless of which drugs they’re using in the operating room,” says Earl Miller, the Picower Professor of Neuroscience and a member of MIT’s Picower Institute for Learning and Memory.
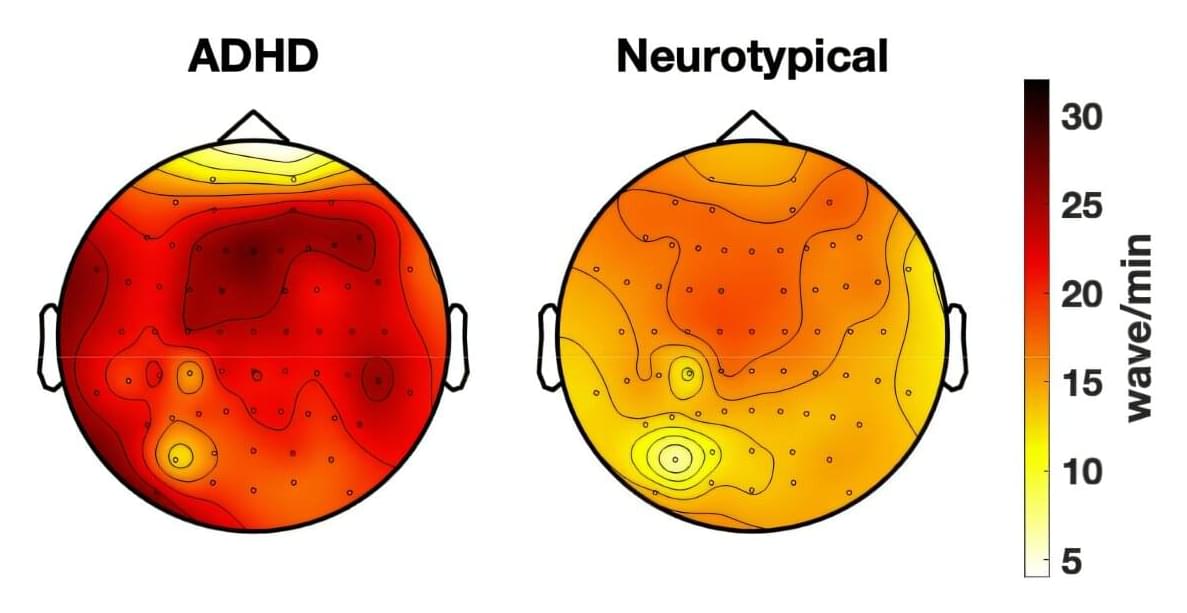
Miller, Edward Hood Taplin Professor of Medical Engineering and Computational Neuroscience Emery Brown, and their colleagues are now working on an automated control system for delivery of anesthesia drugs, which would measure the brain’s stability using EEG and then automatically adjust the drug dose. This could help doctors ensure that patients stay unconscious throughout surgery without becoming too deeply unconscious, which can have negative side effects following the procedure.
Miller and Ila Fiete, a professor of brain and cognitive sciences, the director of the K. Lisa Yang Integrative Computational Neuroscience Center (ICoN), and a member of MIT’s McGovern Institute for Brain Research, are the senior authors of the new study, which appears today in Cell Reports. MIT graduate student Adam Eisen is the paper’s lead author.
Excellent work Earl Miller and team!
Read More