Read a case of anti-Ma2 encephalitis–associated secondary narcolepsy in an elderly man, in whom the diagnosis was delayed because of multiple confounders, but the sleep study was crucial to suspect the final diagnosis.
Background and Objectives.

Children whose fathers took valproate within three months prior to conception were more likely to have neurodevelopmental disorders than children of men exposed to lamotrigine or levetiracetam.
Researchers behind a new study believe that it is the first to show an increased risk of neurodevelopmental disorders in offspring of fathers who took valproate rather than lamotrigine or levetiracetam prior to conceiving children.
Children whose fathers took valproate within the three months prior to their conception were more likely to have neurodevelopmental disorders, including autism spectrum disorders, than children of men exposed to lamotrigine or levetiracetam, according to a study published in JAMA Network Open in November.
The European research team—which analyzed medical records from Denmark, Norway, and Sweden—concluded that “health care practitioners should consider the potential risks associated with paternal valproate exposure and discuss alternative treatment options with male patients of reproductive age.” The team also said that “findings should be interpreted with caution due to the heterogeneity in the unadjusted estimates.”
Scientists studying Alzheimer’s in African Americans have uncovered a striking genetic clue that may cut across racial lines. In brain tissue from more than 200 donors, the gene ADAMTS2 was significantly more active in people with Alzheimer’s than in those without it. Even more surprising, this same gene topped the list in an independent study of White individuals. The discovery hints at a common biological pathway behind Alzheimer’s and opens the door to new treatment strategies.
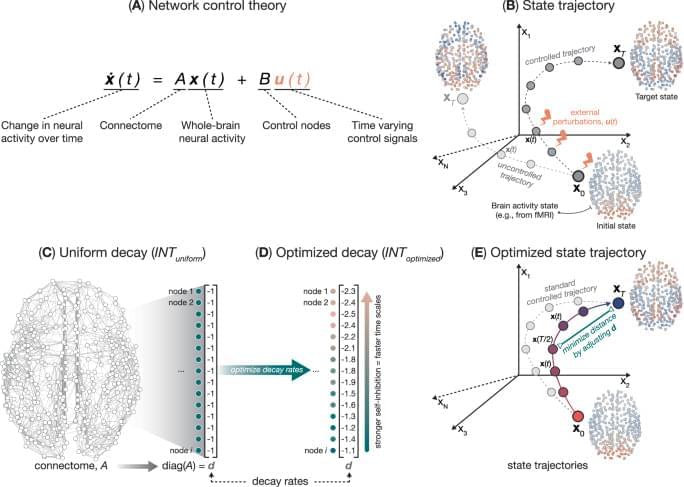
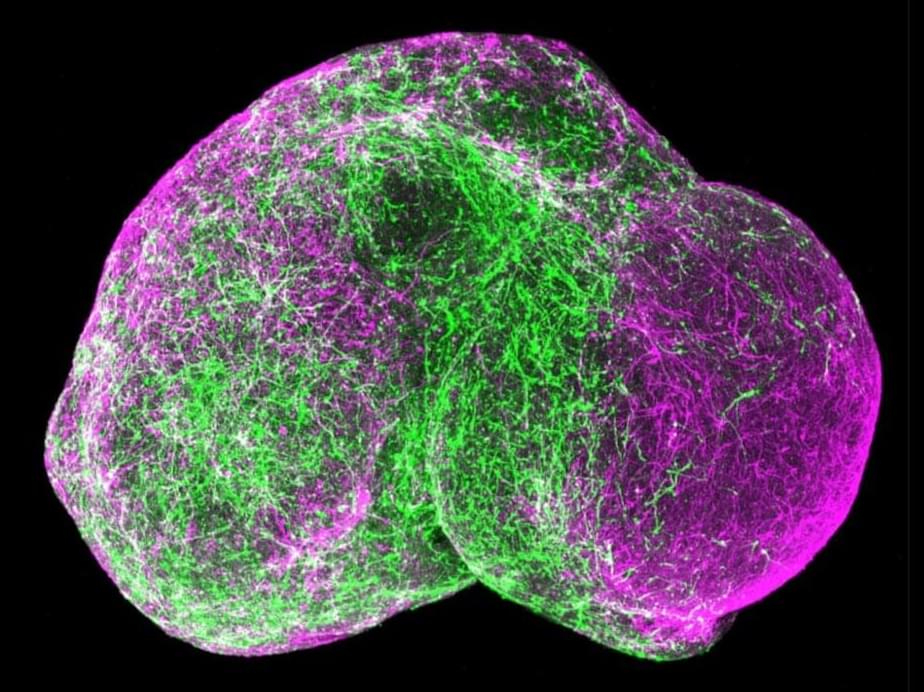

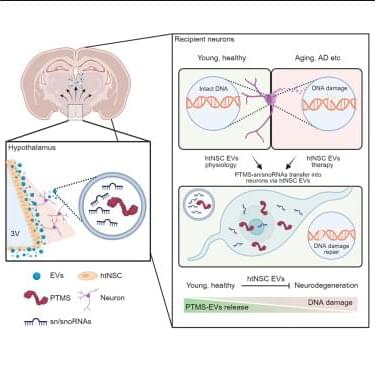
Jung, Yu, Choi et al. reveal a critical neuroprotective role of PTMS, while loss of this protein causes severe neurodegeneration. Hypothalamic neural stem cell-derived extracellular vesicles carrying PTMS protect neurons by preventing DNA damage and offer therapeutic benefits against aging-related neurodegenerative and Alzheimer’s-like conditions in animal models.

From work meetings to first dates, it’s essential to adjust our behavior for success. In certain situations, it can even be a matter of life or death. So how do we switch our behavior when situations change? Published in Nature Communications, neuroscientists describe the neural basis of behavioral flexibility in mice, with insights which may help us understand a wide variety of diseases and disorders, from addiction to obsessive compulsive disorder (OCD) to Parkinson’s disease.
“The brain mechanisms behind changing behaviors have remained elusive, because adapting to a given scenario is very neurologically complex. It requires interconnected activity across multiple areas of the brain,” explains a co-author. “Previous work has indicated that cholinergic interneurons—brain cells that release a neurotransmitter called acetylcholine—are involved in enabling behavioral flexibility. Here, we were able to use advanced imaging techniques to see neurotransmitter release in real time and delve into the fundamental mechanisms behind behavioral flexibility”
In their investigations, the researchers trained mice in a virtual maze, teaching them the correct route to receive a reward. They then switched the route, leading to an unexpected loss of reward for the mice, and observed the effects of this disappointing change using two-photon microscopy.
Yale School of Medicine (YSM) scientists have discovered a molecular difference in the brains of autistic people compared to their neurotypical counterparts.
Autism is a neurodevelopmental condition associated with behavioral differences including difficulties with social interaction, restrictive or intense interests, and repetitive movements or speech. But it’s not clear what makes autistic brains different.
Now, a study in the American Journal of Psychiatry has found that the brains of autistic people have fewer of a specific kind of receptor for glutamate, the most common excitatory neurotransmitter in the brain. The reduced availability of these receptors may be associated with various characteristics linked to autism.