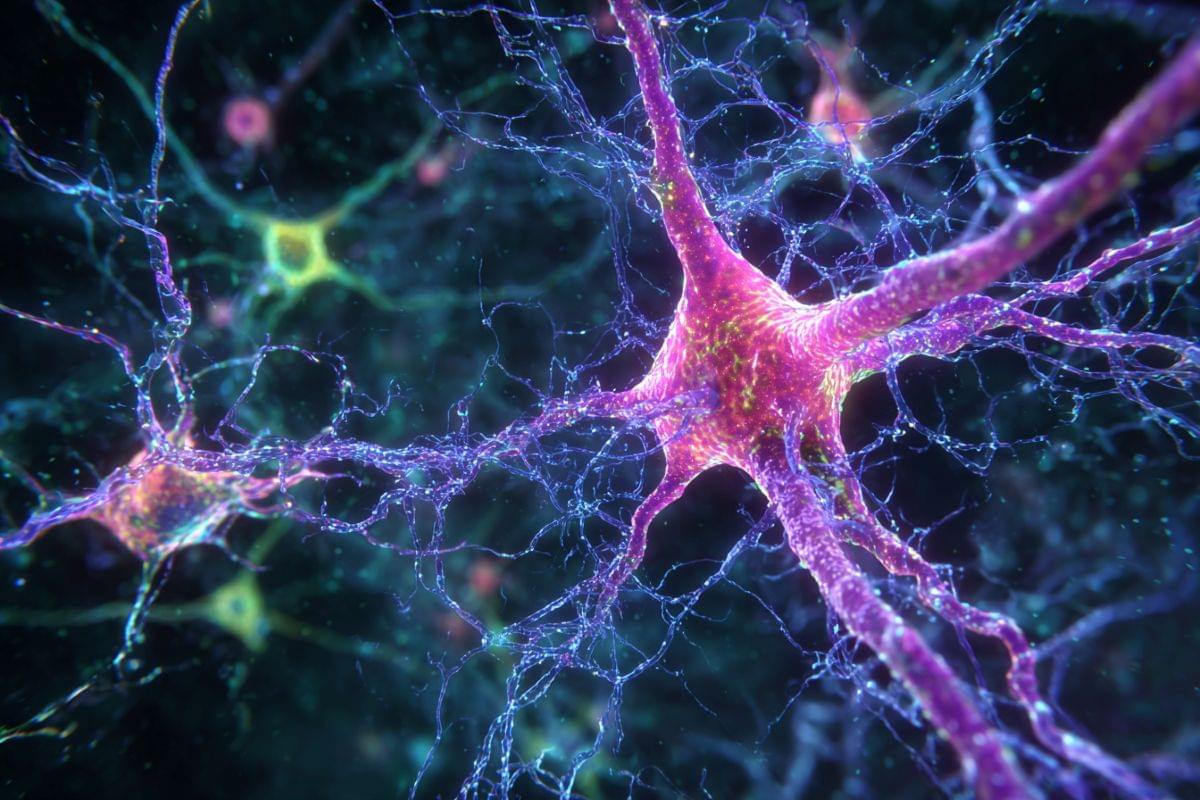
Making a living brain transparent and watching its neurons fire without disturbing their function—sounds like science fiction, doesn’t it? Yet the solution may already exist within our own bodies. In a paper published in Nature Methods, a research team led by Kyushu University introduces a new reagent called SeeDB-Live.
SeeDB-Live uses albumin—a common protein in blood serum—to clear tissue while preserving cellular function. The technique allows scientists to see deeper, brighter structures in both brain slices in a dish and living mice, achieving neural activity that was previously out of sight.
“This is the first time tissue clearing has been achieved without altering its biology,” says Takeshi Imai, professor at Kyushu University’s Faculty of Medical Sciences and the study’s senior author.