The effort to give robots AI brains is revealing big practical challenges—and bigger ethical concerns.


The effort to give robots AI brains is revealing big practical challenges—and bigger ethical concerns.

Artificial intelligence startup Symbolica AI launched today with an original approach to building generative AI models.
The company is aiming to tackle the expensive mechanisms behind training and deploying large language models such as OpenAI’s ChatGPT that are based on Transformer architecture.
Alongside that news, it also revealed today that it has raised $33 million in total funding combined from a Series A and seed funding round led by Khosla Ventures. Other investors included Day One Ventures, Abstract Ventures Buckley Ventures and General Catalyst.

Fascinating vision/plan by the one and only Sam Altman of how to update our economic systems to benefit everyone in the context of rapidly accelerating technological change.
My work at OpenAI reminds me every day about the magnitude of the socioeconomic change that is coming sooner than most people believe. Software that can think and learn will do more and more of the work that people now do. Even more power will shift from labor to capital. If public policy doesn’t adapt accordingly, most people will end up worse off than they are today.
We need to design a system that embraces this technological future and taxes the assets that will make up most of the value in that world–companies and land–in order to fairly distribute some of the coming wealth. Doing so can make the society of the future much less divisive and enable everyone to participate in its gains.
In the next five years, computer programs that can think will read legal documents and give medical advice. In the next decade, they will do assembly-line work and maybe even become companions. And in the decades after that, they will do almost everything, including making new scientific discoveries that will expand our concept of “everything.”
When it comes to achieving success, Huang knows more than most. In 1993, he co-founded computer chip company Nvidia, where he’s served as CEO for more than three decades. The company’s success turned Huang into a billionaire. Now, with Nvidia’s chips in high demand for building AI software, it’s become one of the world’s most valuable companies with a valuation north of $2 trillion.
Huang himself is one of the world’s wealthiest individuals, with an estimated net worth of $77.6 billion, according to Bloomberg.
For Huang, there is one particular trait that can make anyone more likely to become successful: Resilience. At last week’s event, he told Stanford students how he personally developed the resilience necessary to build and run one of the world’s most valuable companies.

The Brazilian Atlantic Rainforest is filled with the ear-piercing ‘screams’ of a tiny amphibian in distress, but until now, we humans have been oblivious to their cries.
For the first time, researchers have recorded South American frogs crying out at a frequency that totally bypasses the human ear – but which would be quite unpleasant to animals with the right kind of receivers.
The leaf litter frog (Haddadus binotatus) is the most abundant species of frog in the forest community. Though abundant, they’re tiny – the largest of the species are females, and even they that barely reach 64 millimeters (2.5 inches) in length.
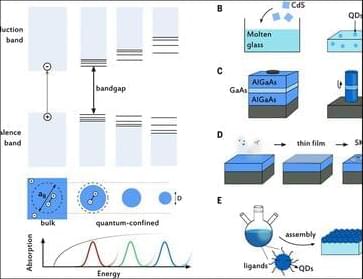
Quantum #dots feature widely tunable and distinctive optical, electrical, chemical, and physical properties. They span energy #harvesting, #ILLUMINATION, #displays, #cameras, and more.
Read more on #WorldQuantumDay: #Sciencereview.
Semiconductor quantum dots: Technological progress and future challenges.

Explore the fun and excitement that comes with Tesla FSD We have curated Tesla FSD test drives, stories, and shorts into a map layout so you can explore how people are trying the Tesla FSD and the reactions they are getting. For best results expand the map to full screen and select from these options.
FSD drives: 66 stories: 14 shorts: 6
If you want to add your FSD adventure video, send us an email to: [email protected] Include the youtube video url, and any comments you want to share smile


