A large international study led by researchers at the Department of Medical Epidemiology and Biostatistics, Karolinska Institutet, shows that major depressive disorder (MDD) not only increases risk for a wide range of diseases and social problems, but is also partly driven by factors such as loneliness, obesity, smoking, and chronic pain.
The study, published in Nature Mental Health, applied genetic methods to systematically test which traits are causes, and which are consequences, of depression. The findings highlight the double burden of MDD: it both arises from and contributes to poor health, making prevention and treatment particularly urgent.
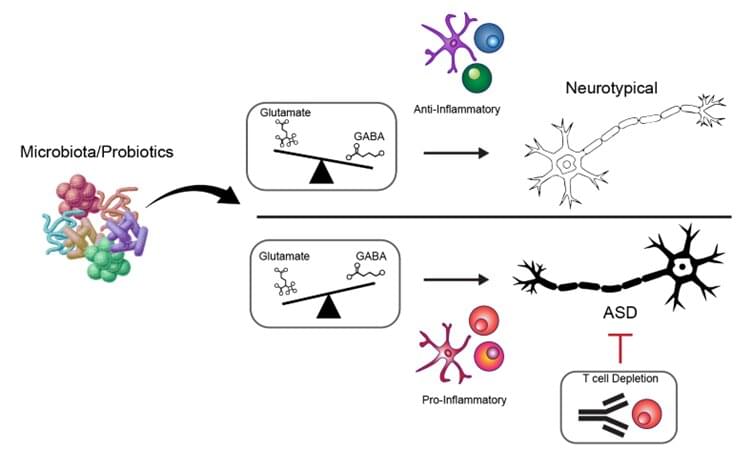
“We show that depression sits at the center of a web of health problems,” says Joëlle Pasman, research associate at Amsterdam UMC and Karolinska Institutet, who led the study. “It is not only a debilitating condition in itself but also increases the risk of many diseases, while at the same time being triggered by social, behavioral, and medical factors.”