Nanobots aren’t just microscopic machines—they could come in countless shapes and sizes, each designed for a unique purpose. From medical nanobots that repair cells to swarming micro-robots that build structures at the atomic level, the future of nanotechnology is limitless. Could these tiny machines revolutionize medicine, industry, and even space exploration? #Nanotech #Nanobots #FutureTech #Science #Innovation …
Category: biotech/medical – Page 674
Childhood Illnesses Surge, Magnetic Poles Wandered, and a Colossal Squid Is Found
Measles cases are going up—and a federal scientist has warned that case counts have probably been underreported. Another vaccine-preventable illness, whooping cough, sees a troubling increase in cases. Ancient humans found sun-protection solutions when Earth’s magnetic poles wandered. A colossal squid has been captured on video in its natural habitat for the first time. Plus, we discuss evidence that Mars once had a carbon cycle and a planet that is orbiting a pair of brown dwarfs.
Episode Transcript: https://www.scientificamerican.com/po… reading: This Is the First Colossal Squid Filmed in the Deep Sea—And It’s a Baby! • See the first colossal squid ever cau… RFK, Jr., Is Wrong about Cause of Rising Autism Rates, Scientists Say https://www.scientificamerican.com/ar… How to Talk about Vaccines in an Era of Scientific Mistrust https://www.scientificamerican.com/ar… E-mail us at [email protected] if you have any questions, comments or ideas for stories we should cover! Discover something new every day: subscribe to Scientific American: https://www.scientificamerican.com/ge… And sign up for Today in Science, our daily newsletter: https://www.scientificamerican.com/ac… Science Quickly is produced by Rachel Feltman, Fonda Mwangi, Kelso Harper, Naeem Amarsy and Jeff DelViscio. This episode was hosted by Rachel Feltman. Our show is edited by Alex Sugiura with fact-checking by Shayna Posses and Aaron Shattuck. The theme music was composed by Dominic Smith.
Recommended reading:
This Is the First Colossal Squid Filmed in the Deep Sea—And It’s a Baby! • See the first colossal squid ever cau…
RFK, Jr., Is Wrong about Cause of Rising Autism Rates, Scientists Say https://www.scientificamerican.com/ar…
How to Talk about Vaccines in an Era of Scientific Mistrust https://www.scientificamerican.com/ar…
E-mail us at [email protected] if you have any questions, comments or ideas for stories we should cover!
Discover something new every day: subscribe to Scientific American: https://www.scientificamerican.com/ge…


Psychedelic use shows minimal link to schizotypal traits with possible reduction in delusional thinking, study suggests
Psychedelic drugs are seeing a surge of interest from mainstream medicine, and initial results suggest that psychedelic-therapy can be a safe and effective treatment for some mental health conditions. However, the side-effect profile is still incompletely understood. In particular, the use of psychedelics has been posited to carry a risk of triggering latent psychotic disorders or persistent visual hallucinations, known as hallucinogen persisting perception disorder (HPPD).
In order to better understand the prevalence and risk factors of such side-effects, Katie Zhou and colleagues surveyed 654 people online who were planning to take psychedelics through their own initiative. The findings are published in the journal PNAS Nexus.
Of the 654 people surveyed, 315 people were resurveyed two weeks after their experience and 212 people were resurveyed again four weeks after their experience. The sample was 74% male, and 77% university-educated. About one-third had been diagnosed with at least one psychiatric condition.

Utilizing ctDNA to discover mechanisms of resistance to targeted therapies in patients with metastatic NSCLC: towards more informative trials
Acquired resistance is a common occurrence among patients with oncogene-driven non-small-cell lung cancer receiving targeted therapies. Monitoring of circulating tumour DNA in liquid biopsy samples provides an appealing, minimally invasive method of monitoring for acquired resistance in this setting. However, research into detecting mechanisms of acquired resistance in liquid biopsy samples has thus far been limited by various challenges. In this Perspective, the authors describe the available data on detecting mechanisms of acquired resistance to targeted therapies in patients with non-small-cell lung cancer, as well as the various challenges to progress, such as a lack of a consensus definition of acquired resistance, and other inconsistencies in the approach to detecting and investigating these alterations.
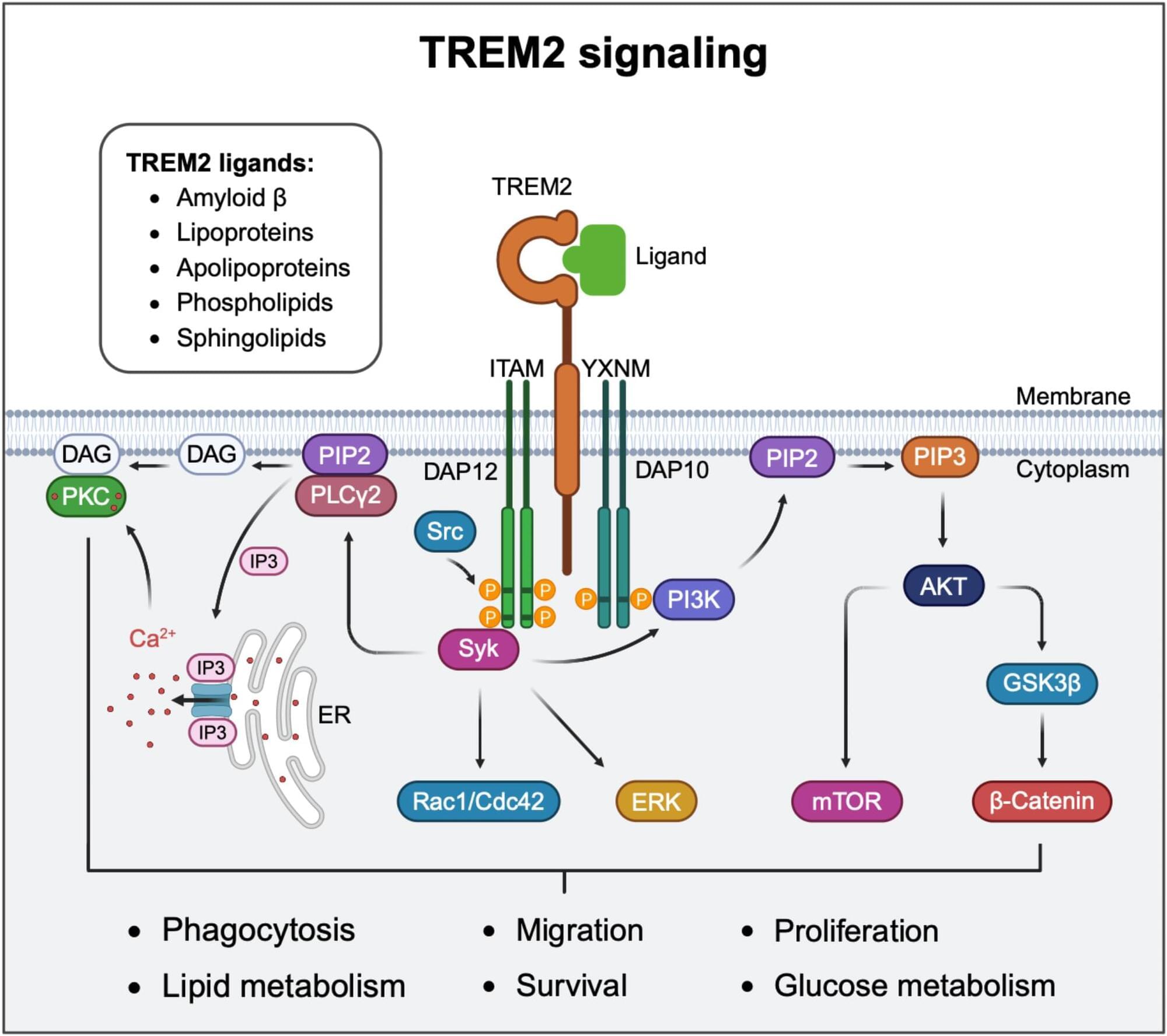
TREM2 and sTREM2 in Alzheimer’s disease: from mechanisms to therapies
The metabolic fitness of microglia is markedly impaired in TREM2 knockout (KO) models [58]. TREM2, through its adaptors DAP12 and DAP10, activates the mechanistic target of rapamycin (mTOR) signaling pathway, which plays a crucial role in regulating metabolic pathways and protein synthesis [11, 58]. Loss of TREM2 impairs mTOR activation, leading to reduced ATP production and biosynthesis. In vivo FDG-PET imaging of TREM2 KO and TREM2 T66M knock-in mice shows a significant reduction in cerebral glucose metabolism [67, 68]. This decrease may correlate with impaired glucose uptake by microglia. Supporting this, ex vivo measurements of isolated microglia from TREM2 KO animals reveal lower FDG uptake [68].
Given the pivotal role of microglial metabolism in AD, targeting this process represents a promising therapeutic strategy. Agents such as interferon-γ (IFN-γ) and cyclocreatine, which enhance ATP production, have been shown to restore microglial functions and mitigate AD pathology [58, 65]. Notably, TREM2-activating antibodies boost microglial energy metabolism by promoting mitochondrial fatty acid and glucose oxidation [69]. Moreover, translocator protein (TSPO)-PET and FDG-PET imaging have demonstrated that TREM2 activation enhances microglial activity and glucose metabolism in amyloid mouse models. Thus, targeting TREM2 and microglial metabolism may complement existing AD therapies, which primarily focus on amyloid clearance and synaptic dysfunction, providing a more comprehensive approach to disease intervention.
Lipid metabolism is crucial for maintaining microglial functions and CNS homeostasis, influencing cellular membrane integrity, energy storage, and inflammatory responses. Emerging evidence identifies TREM2 as a key regulator of lipid metabolism in the brain. TREM2 binds a diverse range of lipids, including anionic and zwitterionic species such as sphingomyelin, phosphatidic acid, phosphatidylinositol, phosphatidylcholine, phosphatidylglycerol, phosphatidylserine (PtdSer) and sulfatide [49, 53, 70]. Among these, PtdSer is the most abundant negatively charged phospholipid in the inner leaflet of the plasma membrane in eukaryotic cells [71]. In neurodegenerative conditions, PtdSer externalization on damaged or apoptotic neurons serves as an “eat-me” signal, triggering TREM2-dependent microglial synaptic pruning and cell clearance [72]. Super-resolution microscopy and in vivo imaging studies have demonstrated that Aβ oligomer-induced hyperactive synapses expose PtdSer, marking them for TREM2-mediated engulfment, which helps mitigate neuronal hyperactivity in AD models. Additionally, individuals carrying TREM2 loss-of-function variants exhibit an accumulation of apoptotic-like synapses [72], underscoring TREM2’s essential role in synaptic homeostasis during early AD pathology. Beyond synaptic pruning, TREM2 facilitates the recognition and clearance of damaged cells. Notably, over-expression of TREM2 in non-phagocytic cells, such as Chinese hamster ovary (CHO) and HEK293 cells, enables them to engulf apoptotic neurons, highlighting TREM2’s function in lipid sensing and phagocytosis [16, 73]. This broad lipid-binding capability underscores TREM2’s critical role in modulating microglial responses to neurodegenerative insults and preserving neuronal health.

Study: Immune therapy works as well in senior cancer patients as in younger adults
It’s well-known that a person’s immune system wears down over time, becoming less effective as folks progress through middle age and become seniors.
But that doesn’t appear to hinder the effectiveness of immunotherapy for cancer in seniors, a new study says.
Seniors with cancer respond just as well as younger patients to immune checkpoint inhibitors — drugs that take the brakes off the immune system so it can target and kill cancer cells more effectively, researchers reported Monday in the journal Nature Communications.

