The simplified edinburgh criteria in clinical practice: a ct-neuropathology accuracy study for diagnosis of cerebral amyloid angiopathy.
Background and Objectives.

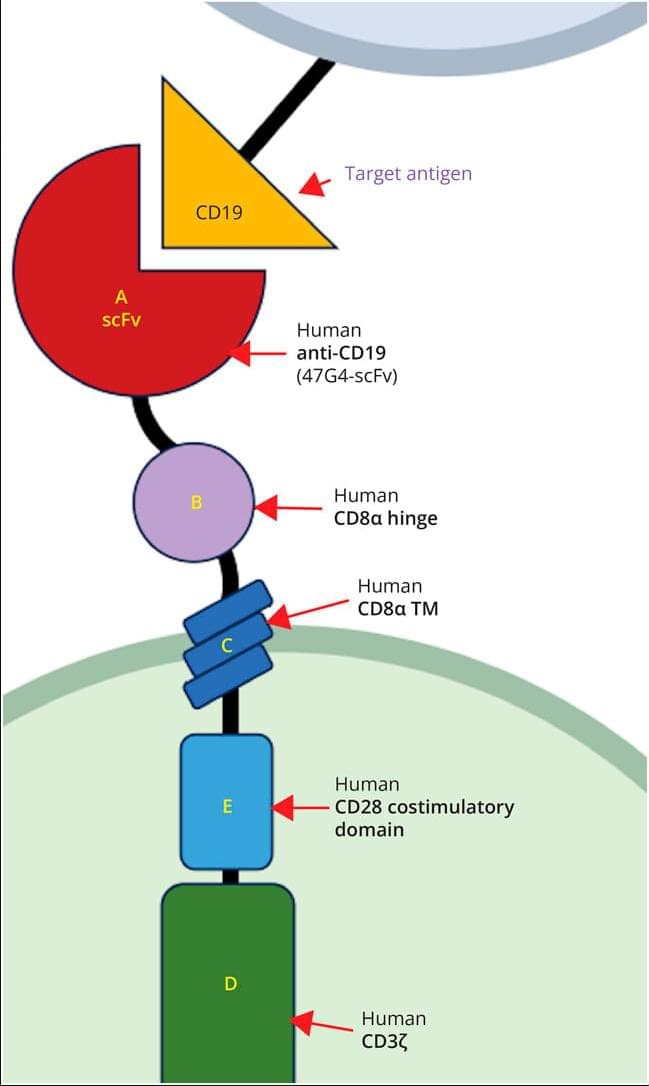
Chimeric antigen receptor (CAR) T cells are genetically modified T cells expressing CARs, initially developed to recognize tumor antigens and kill cancer cells that evade T-cell recognition. Because of their impressive success in hemato-oncologic malignancies, CAR T cells are being repurposed with redesigned constructs for safety and sustained efficacy to target refractory systemic autoimmune or neurologic diseases.

Mitochondrial ATP production by oxidative phosphorylation (OXPHOS) is essential for cellular functions, such that mitochondria are known as the powerhouses of the cell (Verschueren et al., 2019). The mitochondrial ETC consists of five enzyme complexes in the inner membrane of the mitochondria. ETC generates a charge across the inner mitochondrial membrane, which drives ATP synthase (complex V) to synthesize ATP from ADP and inorganic phosphate.
Several studies have shown impairments of all five complexes in multiple areas of the AD brain (Kim et al., 2000, 2001; Liang et al., 2008). Mitochondrial dysfunction in AD is apparent from a decrease in neuronal ATP levels, which is associated with the overproduction of ROS, and indicates that mitochondria may fail to maintain cellular energy. A substantial amount of ATP is consumed in the brain due to the high energy requirements of neurons and glia. Since an energy reserve (such as fat or glucose) is not available in the central nervous system (CNS), brain cells must continuously generate ATP to sustain neuronal function (Khatri and Man, 2013). Mitochondria are the primary source of cellular energy production, but aged or damaged mitochondria produce excess free radicals, which can reduce the supply of ATP and contribute to energy loss and mitochondrial dysfunction in AD. Importantly, oxidative damage of the promoter of the gene encoding subunit of the mitochondrial ATP synthase results in reduced levels of the corresponding protein, leading to decreased ATP production, nuclear DNA damage to susceptible genes, and loss of function (Lu et al., 2004; Reed et al., 2008).
In advanced stages of AD, substantial nitration of ATP synthase subunits can take place, leading to the irregular function of the respiratory chain (Castegna et al., 2003; Sultana et al., 2006; Reed et al., 2009). Likewise, ATP-synthase lipoxidation occurs in the hippocampus and parietal cortex of patients with mild cognitive impairment (Reed et al., 2008). Compromised OXPHOS contributes to a characteristic mitochondrial dysfunction in AD brains, leading to decreased ATP production, elevated oxidative stress, and ultimately cell death (Reddy, 2006; Reddy and Beal, 2008; Du et al., 2012). The specific mechanisms of OXPHOS deficiency in AD remain a long-standing scientific question, but the role of mitochondrial F1Fo ATP synthase dysfunction in AD-related mitochondrial OXPHOS failure is emphasized by emerging evidence (Beck et al., 2016; Gauba et al., 2019).
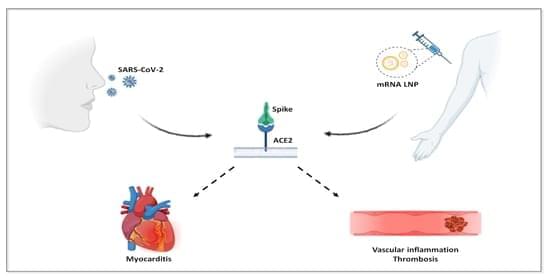
The SARS-CoV-2 (severe acute respiratory syndrome coronavirus responsible for the COVID-19 disease) uses the Spike proteins of its envelope for infecting target cells expressing on the membrane the angiotensin converting enzyme 2 (ACE2) enzyme that acts as a receptor. To control the pandemic, genetically engineered vaccines have been designed for inducing neutralizing antibodies against the Spike proteins. These vaccines do not act like traditional protein-based vaccines, as they deliver the message in the form of mRNA or DNA to host cells that then produce and expose the Spike protein on the membrane (from which it can be shed in soluble form) to alert the immune system. Mass vaccination has brought to light various adverse effects associated with these genetically based vaccines, mainly affecting the circulatory and cardiovascular system.
An injection that blocks the activity of a protein involved in aging reverses naturally occurring cartilage loss in the knee joints of old mice, a Stanford Medicine-led study has found. The treatment also prevented the development of arthritis after knee injuries mirroring the ACL tears often experienced by athletes or recreational exercisers. An oral version of the treatment is already in clinical trials with the goal of treating age-related muscle weakness.
Samples of human tissue from knee replacement surgeries—which include both the extracellular scaffolding, or matrix, in the joint as well as cartilage-generating chondrocyte cells—also responded to the treatment by making new, functional cartilage.
The study results suggest it may be possible to regenerate cartilage lost to aging or arthritis with an oral drug or local injection, rendering knee and hip replacement unnecessary.

Researchers found persistent microclot and NET structures in Long COVID blood that may explain long-lasting symptoms.
Researchers examining Long COVID have identified a structural connection between circulating microclots and neutrophil extracellular traps (NETs). The discovery indicates that the two may interact in the body in ways that could lead to harmful effects when these processes become unregulated.
Understanding Microclots

A discovery from Australian researchers could lead to better treatment for children with neuroblastoma, a cancer that currently claims 9 out of 10 young patients who experience recurrence. The team at the Garvan Institute of Medical Research in Sydney, Australia, found a drug combination that can bypass the cellular defenses these tumors develop that lead to relapse.
In findings made in animal models and published today in Science Advances, Associate Professor David Croucher and his team have shown that a drug already approved for other cancers can trigger neuroblastoma cell death through alternative pathways when the usual routes become blocked. This discovery could lead to better treatment strategies for children whose cancers have stopped responding to standard chemotherapy.
Neuroblastoma is the most common solid tumor in children outside the brain, developing from nerve cells in the adrenal glands above the kidneys or along the spine, chest, abdomen or pelvis. It is typically diagnosed in children under 2 years old. While those with low-risk disease have excellent outcomes, around half of patients are diagnosed with high-risk neuroblastoma—an aggressive form where tumors have already spread. Of these high-risk patients, 15% don’t respond to initial treatment, and half of those who do respond will see their cancer return.


Diabetic kidney disease (DKD) is the leading cause of end-stage renal disease; however, few biomarkers of its early identification are available. The aim of the study was to assess new biomarkers in the early stages of DKD in type 2 diabetes mellitus (DM) patients. This cross-sectional pilot study performed an integrated metabolomic profiling of blood and urine in 90 patients with type 2 DM, classified into three subgroups according to albuminuria stage from P1 to P3 (30 normo-, 30 micro-, and 30 macroalbuminuric) and 20 healthy controls using high-performance liquid chromatography and mass spectrometry (UPLC-QTOF-ESI MS). From a large cohort of separated and identified molecules, 33 and 39 amino acids and derivatives from serum and urine, respectively, were selected for statistical analysis using Metaboanalyst 5.0. online software.