Beware, bad guys—your DNA is in the air.


Summary: ChatGPT has successfully passed a radiology board-style exam, demonstrating the potential of large language models in medical contexts. The study utilized 150 multiple-choice questions mimicking the style and difficulty of the Canadian Royal College and American Board of Radiology exams.
ChatGPT, based on the GPT-3.5 model, answered 69% of questions correctly, just under the passing grade of 70%. However, an updated version, GPT-4, managed to exceed the passing threshold with a score of 81%, showcasing significant improvements, particularly in higher-order thinking questions.
Summary: A new study discovered not all microglia are the same, challenging existing beliefs. A unique subset of these cells, the ARG1+microglia, important for proper cognitive functions, were identified in mice, with evidence suggesting a similar subset exists in humans.
Microglia lacking the protein ARG1 led to less exploratory behavior in mice, indicating cognitive deficits. These discoveries open exciting new possibilities for understanding brain diseases and developing novel therapies.

NewLimit, a company working towards the radical extension of human healthspan using epigenetic reprogramming has announced it has secured $40 million in Series A funding from prominent investors including Dimension, Founders Fund, and Kleiner Perkins.
This investment further bolsters the company’s belief that therapies to delay, halt or even reverse aging can be found through the exploration of epigenetic reprogramming. With a strong belief that their innovative approach can also address various age-related diseases, NewLimit aims to revolutionize the field of aging biology and pave the way for transformative advancements in healthcare.
Longevity. Technology: Epigenetic reprogramming is an emerging but exciting field of geroscience. It involves the identification of specific sets of transcription factors that can induce changes in gene expression and cellular behavior, effectively reversing or modifying the epigenetic markers associated with aging. This approach offers a unique opportunity to rejuvenate cells and tissues, potentially slowing down or even reversing the effects of aging and its related diseases. NewLimit says that while its products are designed to treat aging itself, the company also believes “these products could treat or prevent many diseases associated with aging, including fibrosis, infectious disease, and neurodegenerative disease.”
A new publication in the May issue of Nature Aging by researchers from Integrated Biosciences, a biotechnology company combining synthetic biology and machine learning to target aging, demonstrates the power of artificial intelligence (AI) to discover novel senolytic compounds, a class of small molecules under intense study for their ability to suppress age-related processes such as fibrosis, inflammation and cancer.
The paper, “Discovering small-molecule senolytics with deep neural networks,” authored in collaboration with researchers from the Massachusetts Institute of Technology (MIT) and the Broad Institute of MIT and Harvard, describes the AI-guided screening of more than 800,000 compounds to reveal three drug candidates with comparable efficacy and superior medicinal chemistry properties than those of senolytics currently under investigation.
“This research result is a significant milestone for both longevity research and the application of artificial intelligence to drug discovery,” said Felix Wong, Ph.D., co-founder of Integrated Biosciences and first author of the publication. “These data demonstrate that we can explore chemical space in silico and emerge with multiple candidate anti-aging compounds that are more likely to succeed in the clinic, compared to even the most promising examples of their kind being studied today.”

Dr. Steven Gazal, an assistant professor of population and public health sciences at the Keck School of Medicine of USC, is on a mission to answer a perplexing question: Why, despite millions of years of evolution, do humans still suffer from diseases?
As part of an international research team, Gazal has made a groundbreaking discovery. They’ve become the first to accurately pinpoint specific base pairs in the human genome that have remained unaltered throughout millions of years of mammalian evolution. These base pairs play a significant role in human disease. Their findings were published in a special Zoonomia edition of the journal Science.
Gazal and his team analyzed the genomes of 240 mammals, including humans, zooming in with unprecedented resolution to compare DNA.


We’re currently working with companies that develop software and tools that make surgery smarter and safer while they empower surgeons and providers to improve patient outcomes, enhance operational efficiency and increase profitability with data-driven surgery using AI, automation and operating room analytics. This is where analytic components such as data lakes and warehouses are already making a difference in healthcare. We’ve seen them capable of powering millions of facts and patient records at a time. Tied to expertise, these tools allow data-informed decisions for measurable improvements in clinical, financial and operational aspects.
For instance, we’ve helped design and develop surgical applications to improve operating room efficiency, tele-surgery, data lake construction and surgical analytics. Clients come back with feedback on our skills and technical experience, feeling supported by the flexibility and technical boost we give their teams.
Collaboration between technology outsourcing companies and healthcare providers can result in considerable optimization, including improved patient care and maximized processes. Tech providers can strive for the perfect collaborative balance with the above key conversations while boosting robust ecosystems, shared platforms and data.
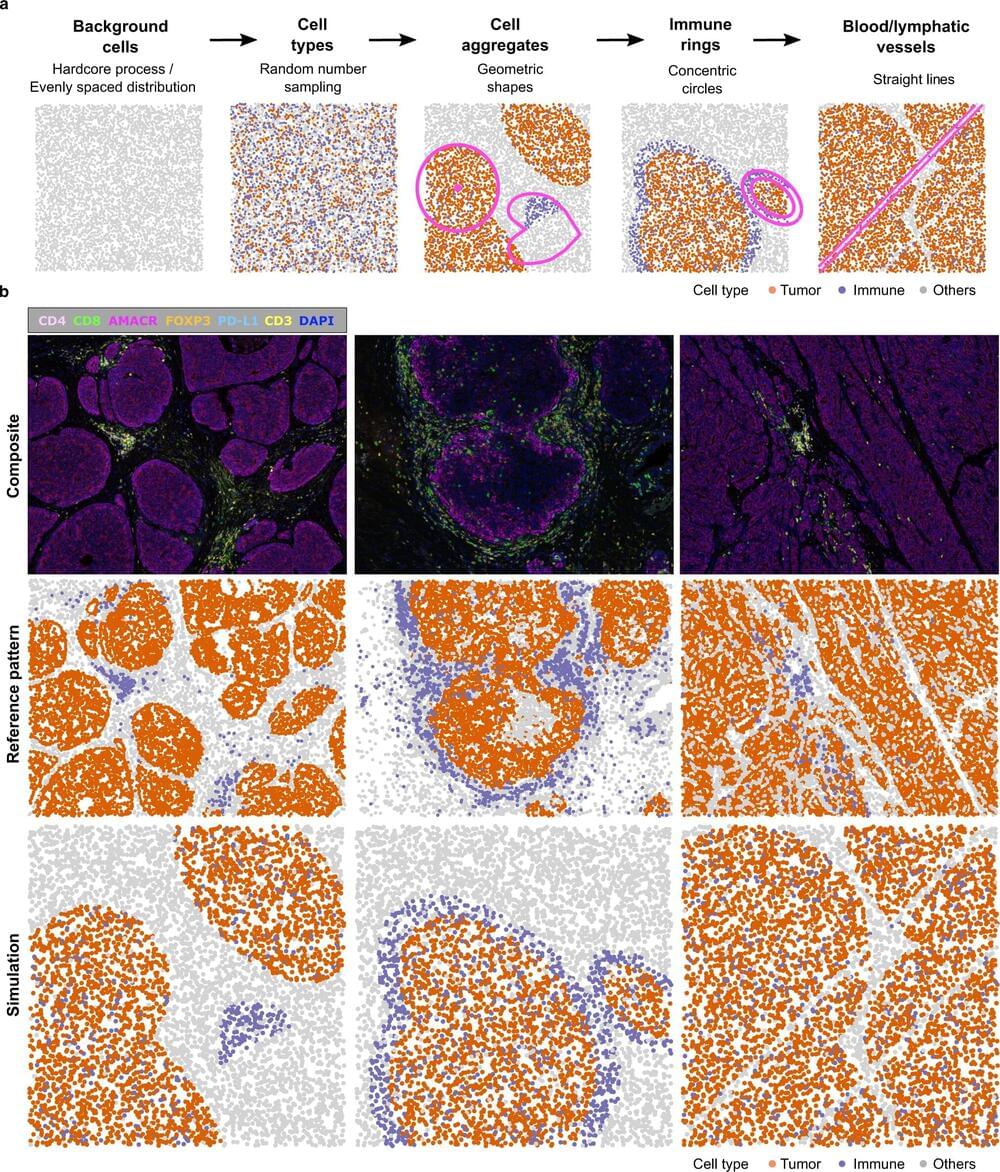
Research published in Nature Communications today, has shown that techniques initially developed for astronomy and ecology can be used to study the microenvironment of solid tumors.
Led by Peter Mac’s 2020 Lea Medal winner Dr. Anna Trigos and Yuzhou Feng, the study looked at patient tumor samples from prostate, colon and breast cancers and identified novel cancer subtypes, new patterns associated with patient survival, and was able to predict which patients were likely to develop metastasis first.
These exciting results have generated significant interest from medical oncologists, pathologists and immunologists.