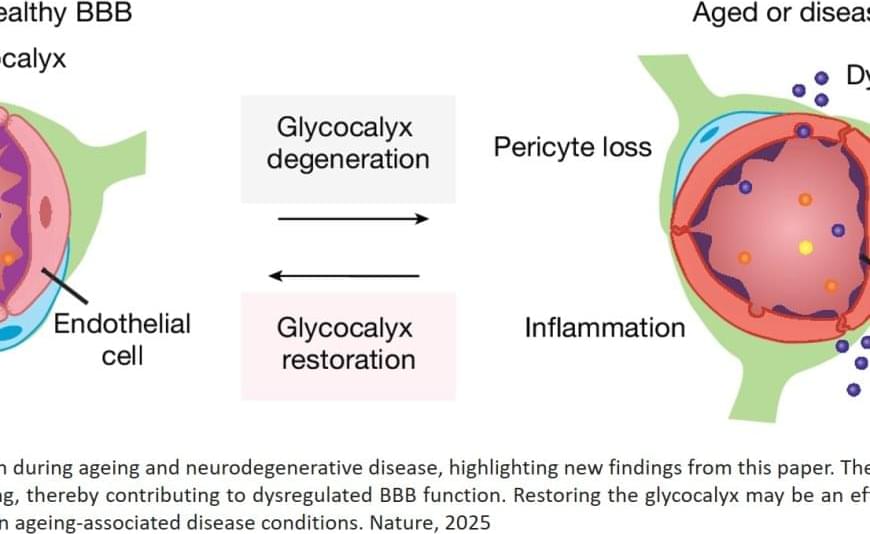
In a study in aging mice, the first author has uncovered striking age-related changes in the sugary coating – called the glycocalyx – on cells that form the blood-brain barrier, a structure that protects the brain by filtering out harmful substances while allowing in essential nutrients.
“The glycocalyx is like a forest,” the author explains. “In young, healthy brains, this forest is lush and thriving. But in older brains, it becomes sparse, patchy, and degraded.”
These age-related changes to the glycocalyx weaken the blood-brain barrier, the author found. As the barrier becomes leaky with age, harmful molecules can infiltrate the brain, potentially fueling inflammation, cognitive decline, and neurodegenerative diseases.
The results were striking: In older mice, bottlebrush-shaped, sugar-coated proteins called mucins, a key component of the glycocalyx, were significantly reduced. This thinning of the glycocalyx correlated with increased permeability of the blood-brain barrier and heightened neuroinflammation.
When the team reintroduced those critical mucins in aged mice, restoring a more “youthful” glycocalyx, they improved the integrity of the blood-brain barrier, reduced neuroinflammation, and measurably improved cognitive function.
“Modulating glycans has a major effect on the brain – both negatively in aging, when these sugars are lost, and positively, when they are restored,” the lead says. “This opens an entirely new avenue for treating brain aging and related diseases.”