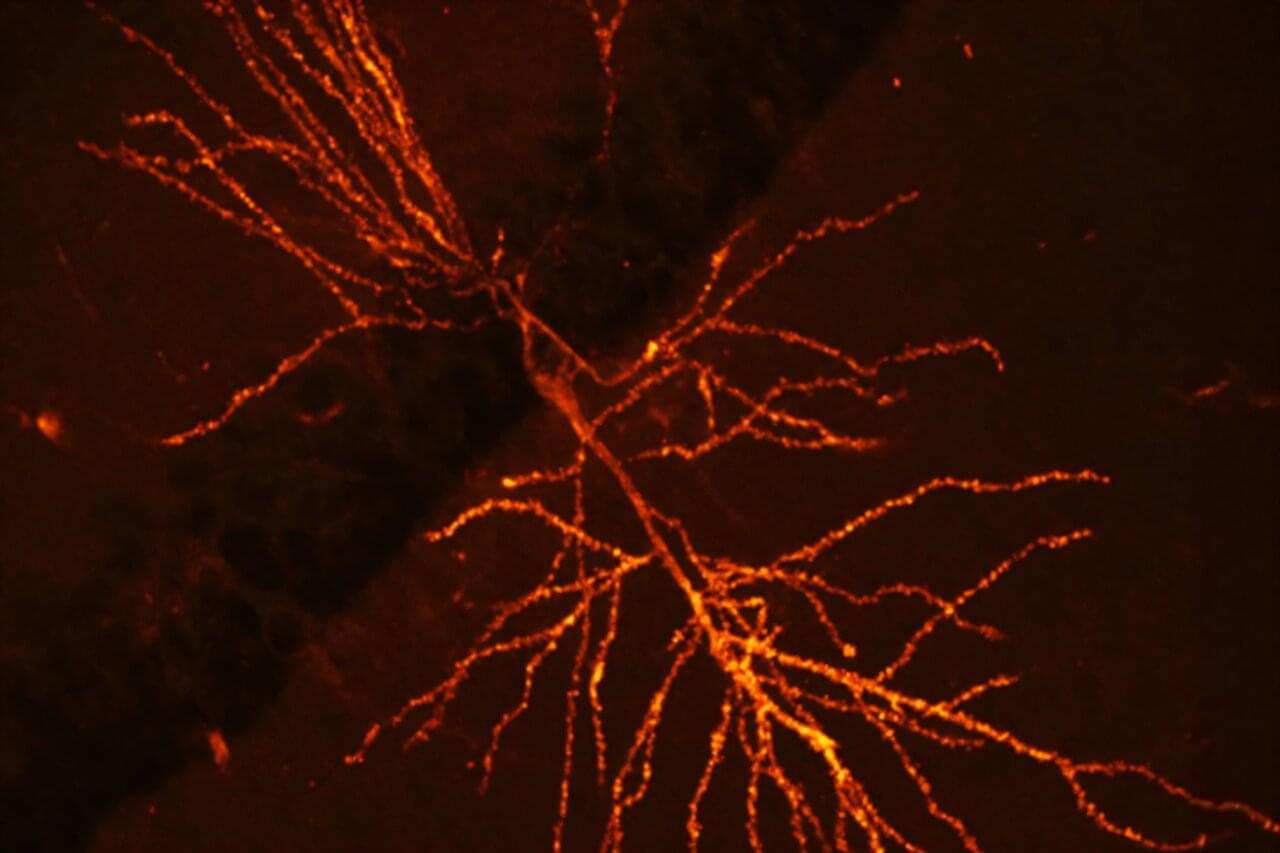
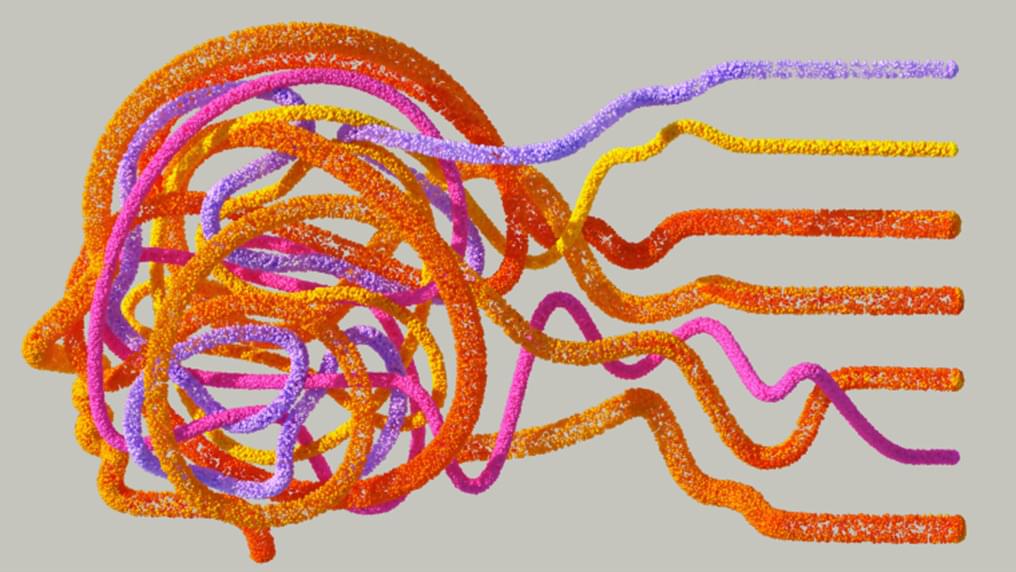
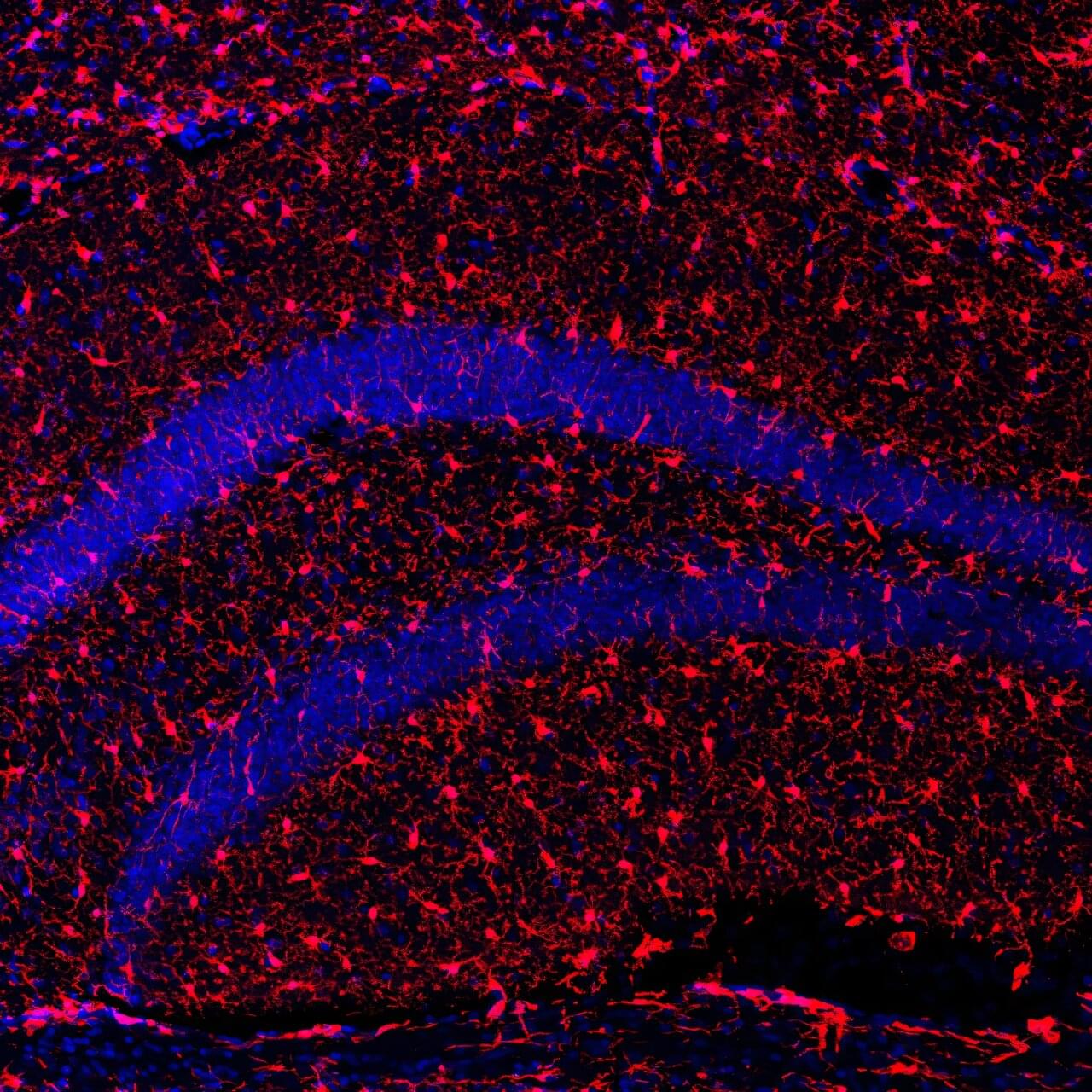
Our brain is a complex organ. Billions of nerve cells are wired in an intricate network, constantly processing signals, enabling us to recall memories or to move our bodies.
Making sense of this complicated network requires a precise look into how these nerve cells are arranged and connected. “LICONN,” a new microscopy method developed by scientists at the Institute of Science and Technology Austria (ISTA) and Google Research, now helps piece together this puzzle.
Light microscopes have been evolving for centuries. Scientists use light microscopy to—literally and figuratively—illuminate the most intricate biological structures. However, unraveling the complex details and architecture of the brain remains a seemingly impossible challenge, considering its billions of densely packed neurons, each linked to other cells via thousands of synapses.