A large meta-analysis of 25 studies found that people with anxiety disorders have significantly lower levels of choline, a vital brain nutrient, compared to individuals without anxiety.

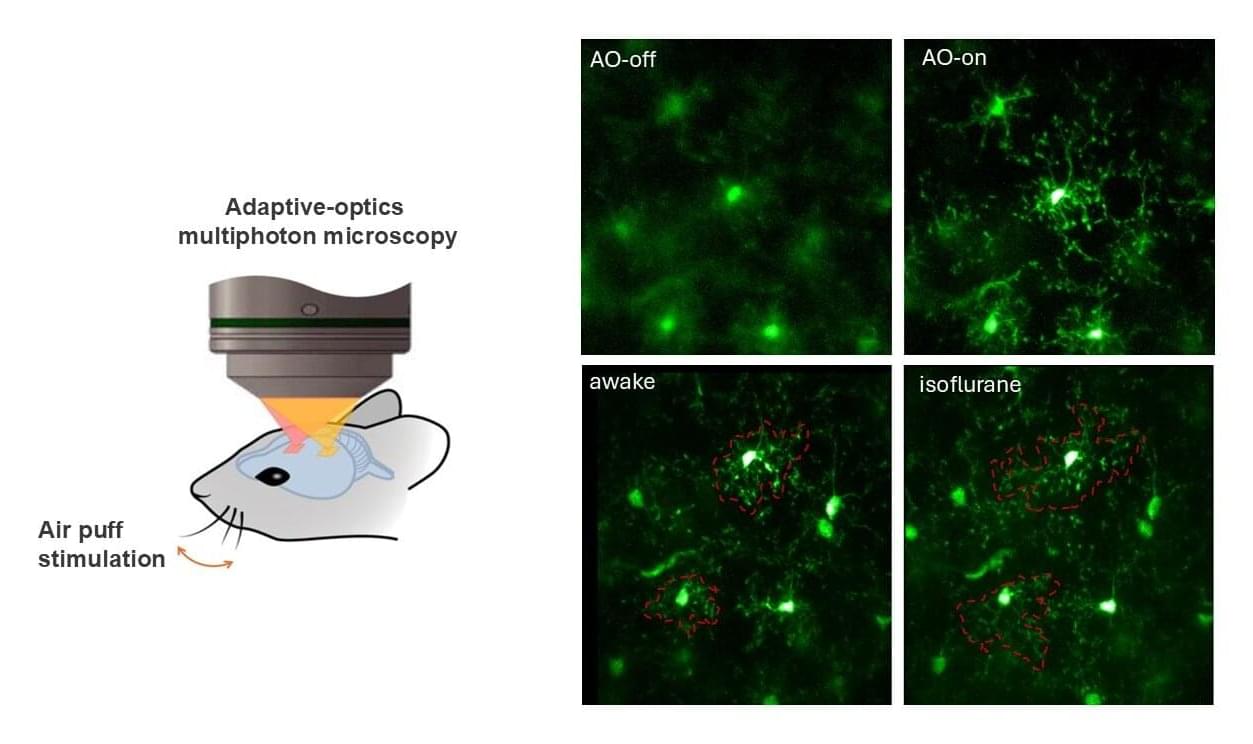
A research team from the School of Engineering at The Hong Kong University of Science and Technology (HKUST) has achieved a breakthrough in brain imaging by developing the world’s first technology to capture high-resolution images of the brains of awake experimental mice in a nearly noninvasive manner.
By eliminating the need for anesthesia, this innovation enables scientists to study brain tissue in its fully functional state. The advancement promises deeper insights into human brain function in both healthy and diseased conditions, opening new frontiers in neuroscience research.
The study was recently published in Nature Communications in a paper titled “Rapid adaptive optics enabling near-noninvasive high-resolution brain imaging in awake behaving mice.”

Meditation, and Open Label Placebo Healing Intervention in the scientific journal Communications Biology.
The landmark study demonstrates how intensive meditation can trigger the same profound brain activity previously documented only with psychedelic substances – while simultaneously activating measurable biological transformations throughout the entire body.


Creatures like sea stars, jellyfish, sea urchins and sea anemones don’t have brains, yet they can capture prey, sense danger and react to their surroundings.
So does that mean brainless animals can think?
“Brainless does not necessarily mean neuron-less,” Simon Sprecher, a professor of neurobiology at the University of Fribourg in Switzerland, told Live Science in an email. Apart from marine sponges and the blob-like placozoans, all animals have neurons, he said.
Creatures like jellyfish, sea anemones and hydras possess diffuse nerve nets — webs of interconnected neurons distributed throughout the body and tentacles, said Tamar Lotan, head of the Cnidarian Developmental Biology and Molecular Ecology Lab at the University of Haifa in Israel.
“The nerve net can process sensory input and generate organized motor responses (e.g., swimming, contraction, feeding, and stinging), effectively performing information integration without a brain,” she told Live Science in an email.
This simple setup can support surprisingly advanced behavior. Sprecher’s team showed that the starlet sea anemone (Nematostella vectensis) can form associative memories — learning to link two unrelated stimuli. In the experiment, the researchers trained sea anemones to associate a harmless flash of light with a mild shock. Eventually, the light alone made them retract.
Another experiment showed that sea anemones can learn to recognize genetically identical neighbors after repeated encounters and curb their usual territorial aggression. The fact that anemones change their behavior toward genetically identical neighbors suggests they can distinguish between “self” and “non-self”
The researchers said they have completed a first draft of atlases of the developing human brain and the developing mammalian brain.
The research focused on human and mouse brain cells, with some work in monkey brain cells too. In their initial draft, the scientists mapped the development of different types of brain cells — tracking how they are born, differentiate and mature into various types with unique functions. They also tracked how genes are turned on or off in these cells over time.
The scientists identified key genes controlling brain processes and uncovered some commonalities of brain cell development between human and animal brains, as well as some unique aspects of the human brain, including identifying previously unknown cell types.
Scientists have reached a milestone in an ambitious initiative to chart how the many types of brain cells emerge and mature from the earliest embryonic and fetal stages until adulthood, knowledge that could point to new ways of tackling certain brain-related conditions like autism and schizophrenia.

This is the conclusion of an international team of researchers, who found that this nervous system has a genetic organization resembling that of the brain of vertebrates, like humans.
“Our results show that animals without a conventional central nervous system can still develop a brainlike organization,” said paper author and biologist Jack Ullrich-Lüter of the Natural History Museum, Berlin, in a statement.
He added: “This fundamentally changes how we think about the evolution of complex nervous systems.”

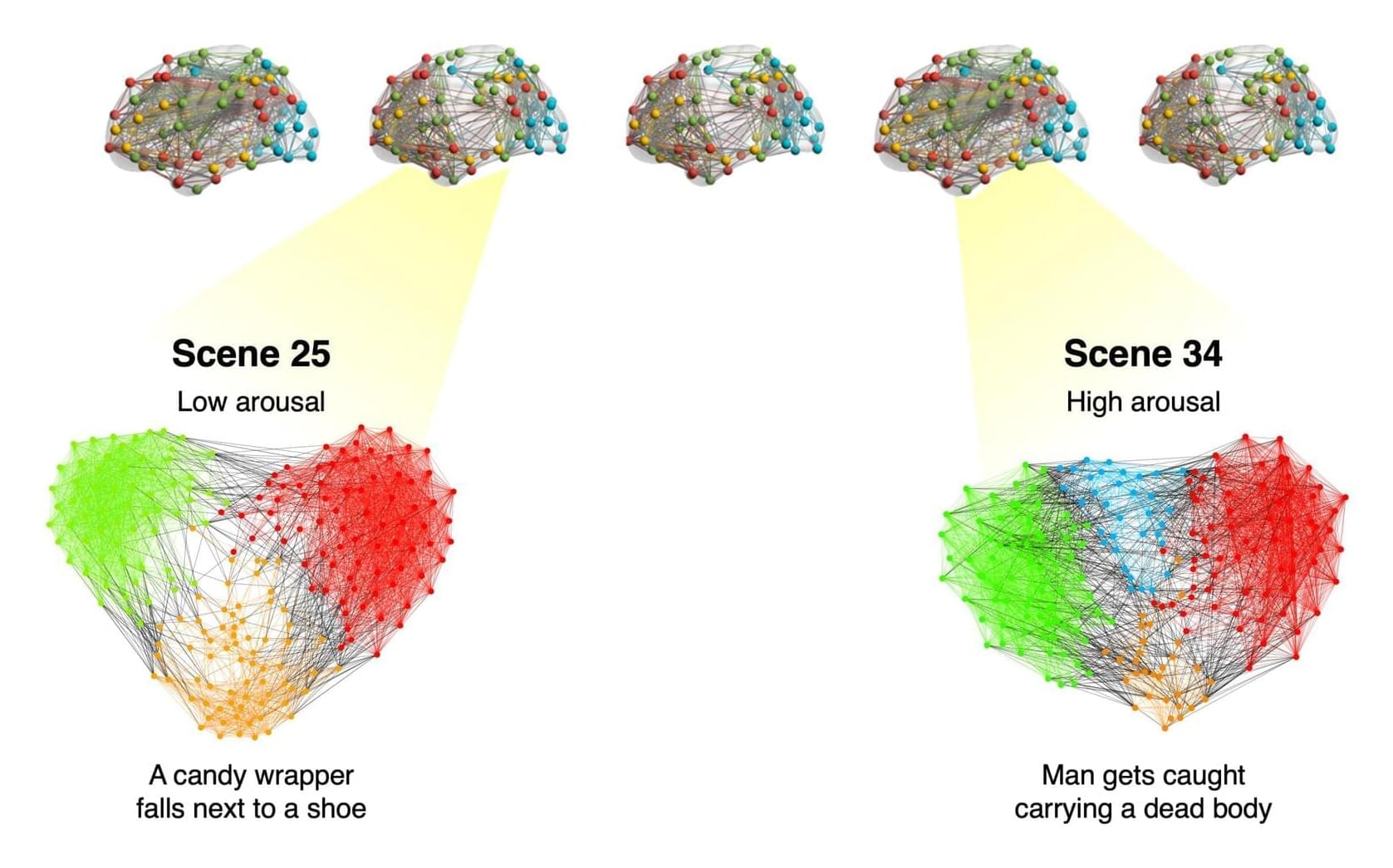
Past psychology studies suggest that people tend to remember emotional events, such as their wedding, the birth of a child or traumatic experiences, more vividly than neutral events, such as a routine professional meeting. While this link between emotion and the recollection of past events is well-established, the neural mechanisms via which emotional states strengthen memories remain poorly understood.
Researchers at the University of Chicago and other institutes carried out a study aimed at better understanding these mechanisms. Their findings, published in Nature Human Behaviour, suggest that emotional states facilitate the encoding of memories by increasing communication between networks of brain regions.
“Emotional experiences tend to be ‘sticky,’ meaning that they endure in our memories and shape how we interpret the past, engage with the present, and anticipate the future,” Yuan Chang Leong, senior author of the paper, told Medical Xpress.