“Researchers at George Washington University have linked fast-food consumption to the presence of potentially harmful chemicals, a connection they argue could have “great public health significance.””


“Researchers at George Washington University have linked fast-food consumption to the presence of potentially harmful chemicals, a connection they argue could have “great public health significance.””

Imagine shirts that act as antennas for smartphones or tablets, workout clothes that monitor fitness level or even a flexible fabric cap that senses activity in the brain!
All this will soon be possible as the researchers working on wearable electronics have been able to embroider circuits into fabric with super precision — a key step toward the design of clothes that gather, store or transmit digital information.
“A revolution is happening in the textile industry. We believe that functional textiles are an enabling technology for communications and sensing and one day, even for medical applications like imaging and health monitoring,” said lead researcher John Volakis from Ohio State University.

The discomfort and stigma of loose or missing teeth could be a thing of the past as Griffith University researchers pioneer the use of 3D bioprinting to replace missing teeth and bone.
The three-year study, which has been granted a National Health and Medical Research Council Grant of $650,000, is being undertaken by periodontist Professor Saso Ivanovski from Griffith’s Menzies Health Institute Queensland.
As part of an Australian first, Professor Ivanovski and his team are using the latest 3D bioprinting to produce new, totally ‘bespoke,’ tissue engineered bone and gum that can be implanted into a patient’s jawbone.
VR is Poised to Change Many Facets of Healthcare. Find out How.

#nutrition #CrapScience
So after 40 years of prescribing low fat diets & demonising cholesterol, the largest & longest clinical experiment ever (40 years, 9,000 patients, randomly assigned diets) shows that “Patients who lowered their cholesterol, presumably because of the special diet, actually suffered MORE heart-related deaths than those who did not.”
In other words, if you’ve been cutting on steaks, butter etc. for 4 years or more, you may have INCREASED your mortality rate from heart disease by %8.
Oops?
Via Oxford Martin School @oxmartinschool
A fuller accounting of the results of a massive government-funded experiment on fatty foods challenges the conventional advice about what is healthy, and what is not.
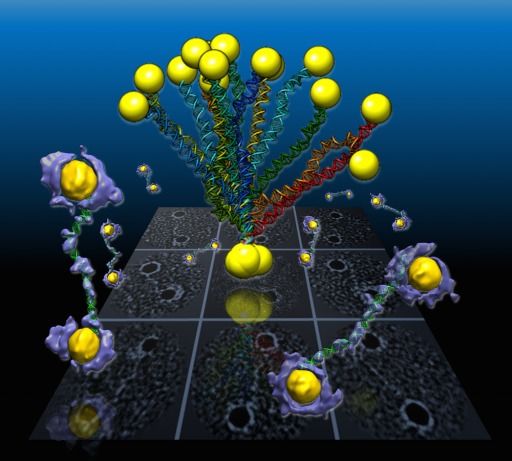
“DNA base pairing has been used for many years to direct the arrangement of inorganic nanocrystals into small groupings and arrays with tailored optical and electrical properties. The control of DNA-mediated assembly depends crucially on a better understanding of three-dimensional structure of DNA-nanocrystal-hybridized building blocks. Existing techniques do not allow for structural determination of these flexible and heterogeneous samples.”

My own prediction is that we will see singularity with humans 1st via BMI/ BI technology and other bio-computing technology before we see a machine brain operating a the level of a healthy fully funtional human brain.
Since War of the Worlds hit the silver screen, never has the notion that machine intelligence will overtake human intelligence is more real. In this two-part series, the author examines the growing trend towards cognitive machines.
It might be time to rethink fertility treatment.
Here’s the scoop: scientists at Northwestern University 3D printed a functional ovary out of Jello-like material and living cells. When implanted into mice that had their ovaries removed, the moms regained their monthly cycle and gave birth to healthy pups.
The scientists presented their results last week at the Endocrine Society’s annual meeting in Boston.

A major concerned for Lockheed is the long passage of time between the crew’s training and the moment a serious issue does come up during a mission—which could be a few years later. “They may not remember the training. Having the right kind of on-board documentation and flight computer to be able to provide the astronauts the information they need when they need it, is important,” Pratt said. “Not just having the alarm go off but having the alarm go off and the PDF file of the manual come up at the same time. That’s really useful in helping the crew understand how to operate their own vehicle.”
Even though Lockheed Martin’s early habitat concept will service exploration missions near the Moon, the company is always thinking about the manned mission to Mars, which will require a far more advanced successor to their current designs. Engineers will need to go through a few iterations of the concept after the health effects of long-duration human spaceflight are known and as new technology is developed. This is the basis that NASA created NextSTEP on.
The federal space agency is looking for a modular habitat that can grow, evolve and be added to. “New modules are built upon the lessons of the previous modules,” Hopkins said.
Very cool.
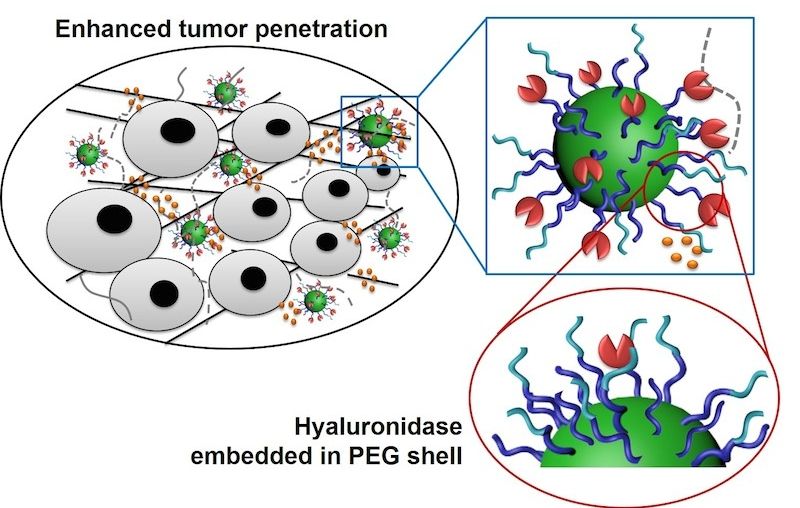
For more than a decade, biomedical researchers have been looking for better ways to deliver cancer-killing medication directly to tumors in the body. Tiny capsules, called nanoparticles, are now being used to transport chemotherapy medicine through the bloodstream, to the doorstep of cancerous tumors. But figuring out the best way for the particles to get past the tumor’s “velvet rope” and enter the tumor is a challenge scientists are still working out. Drexel University researchers believe that the trick to gaining access to the pernicious cellular masses is to give the nanoparticles a new look—and that dressing to impress will be able to get them past the tumor’s biological bouncers.
Targeted cancer therapy is most effective when the medication is released as close as possible to the interior of a tumor, to increase its odds of penetrating and killing off cancerous cells. The challenge that has faced cancer researchers for years is making a delivery vehicle that is sturdy enough to safely get the medication through the bloodstream to tumors—which is no smooth ride—but is also lithe enough to squeeze through the tumor’s dense extra cellular space—a matrix stuffed with sugars called hyaluronic acid.
In research recently published in the journal Nano Letters, lead author Hao Cheng, PhD, an assistant professor with an appointment in Drexel’s College of Engineering, and affiliation with School of Biomedical Engineering, Science and Health Systems; reports that the way to get past the tumor’s front door has everything to do with how the tiny particle is suited up for the journey.