Neurons produced from frontotemporal dementia patients’ skin biopsies using modern stem cell technology recapitulate the synaptic loss and dysfunction detected in the patients’ brains, a new study from the University of Eastern Finland shows.
Frontotemporal dementia is a progressive neurodegenerative disease affecting the frontal and temporal lobes of the brain. The most common symptoms are behavioral changes, difficulties in understanding or producing speech, problems in movement, and psychiatric symptoms. Often, frontotemporal dementia has no identified genetic cause, but especially in Finnish patients, hexanucleotide repeat expansion in the C9orf72 gene is a common genetic cause, present in about half of the familial cases and in 20 per cent of the sporadic cases where there is no family history of the disease. However, the disease mechanisms of the different forms of frontotemporal dementia are still poorly understood, and there are currently no effective diagnostic tests or treatments affecting the progression of the disease in clinical use.
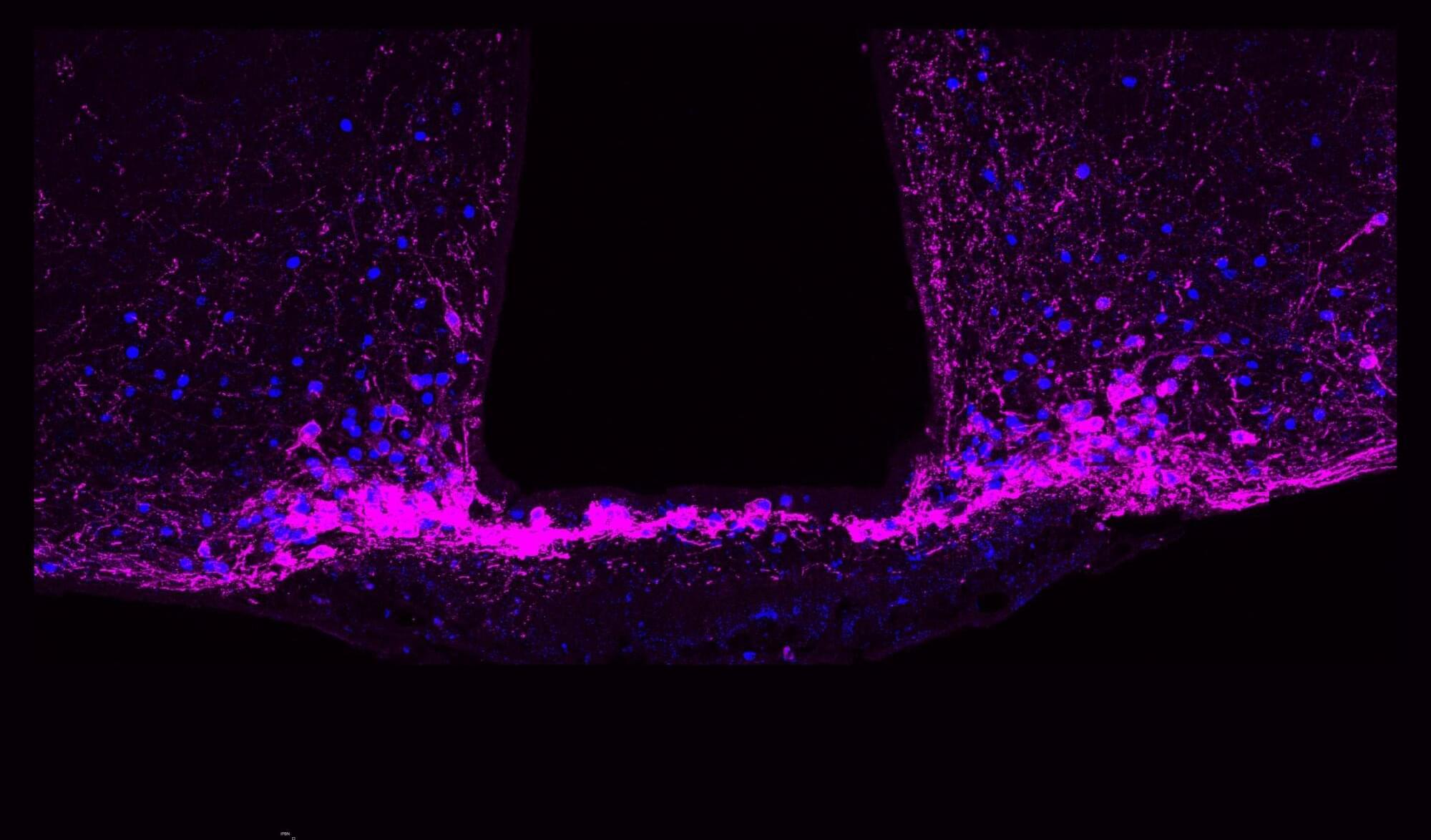
Brain imaging and neurophysiological studies have shown that pathological and functional changes underlying the symptoms occur at synapses, the connections between brain neurons, in frontotemporal dementia patients. PET imaging studies have shown significant synapse loss in the brain, and transcranial magnetic stimulation, on the other hand, has indicated disturbed function of both excitatory and inhibitory neurotransmitter systems, leading to deficient neurotransmission. Often, drugs affecting the different neurotransmitter systems are used to mitigate the symptoms of frontotemporal dementia patients.