The Human Genome Project promised medical advances from knowledge of the DNA inside nearly every human cell. Now, around 20 years later, nucleic acids — the building blocks of DNA and RNA — are at the centre of powerful approaches to new medicines.


Researchers at the University of Helsinki have uncovered a mechanism that instantaneously generates DNA palindromes, potentially leading to the creation of new microRNA genes from noncoding DNA sequences. This discovery, which was made while studying DNA replication errors and their impact on RNA molecule structures, offers new insights into gene origins.
The complexity of living organisms is encoded within their genes, but where do these genes come from? Researchers at the University of Helsinki resolved outstanding questions around the origin of small regulatory genes, and described a mechanism that creates their DNA palindromes. Under suitable circumstances, these palindromes evolve into microRNA genes.
Genes and proteins: the building blocks of life.

2023 was the year that CRISPR gene-editing sliced its way out of the lab and into the public consciousness—and American medical system. The Food and Drug Administration recently approved the first gene-editing CRISPR therapy, Casgevy (or exa-cel), a treatment from CRISPR Therapeutics and partner Vertex for patients with sickle cell disease. This comes on the heels of a similar green light by U.K. regulators in a historic moment for a gene-editing technology whose foundations were laid back in the 1980s, eventually resulting in a 2020 Nobel Prize in Chemistry for pioneering CRISPR scientists Jennifer Doudna and Emmanuelle Charpentier.
That decades-long gap between initial scientific spark, widespread academic recognition, and now the market entry of a potential cure for blood disorders like sickle cell disease that afflict hundreds of thousands of people around the world is telling. If past is prologue, even newer CRISPR gene-editing approaches being studied today have the potential to treat diseases ranging from cancer and muscular dystrophy to heart disease, birth more resilient livestock and plants that can grapple with climate change and new strains of deadly viruses, and even upend the energy industry by tweaking bacterial DNA to create more efficient biofuels in future decades. And novel uses of CRISPR, with assists from other technologies like artificial intelligence, might fuel even more precise, targeted gene-editing—in turn accelerating future discovery with implications for just about any industry that relies on biological material, from medicine to agriculture to energy.
With new CRISPR discoveries guided by AI, specifically, we can expand the toolbox available for gene editing, which is crucial for therapeutic, diagnostic, and research applications… but also a great way to better understand the vast diversity of microbial defense mechanisms, said Feng Zhang, another CRISPR pioneer, molecular biologist, and core member at the Broad Institute of MIT and Harvard in an emailed statement to Fast Company.
7 month treatment, 6 years returned according to a methylation clock, mostly in people who’s biological age was greater than their calendar age.
Dr. Brian Kennedy presents 4 molecules which show promising effects in both healthspan & lifespan in this video. https://pubmed.ncbi.nlm.nih.gov/37289866/http… https://pubmed.ncbi.nlm.nih.gov/37637… https://pubmed.ncbi.nlm.nih.gov/37925… https://pubmed.ncbi.nlm.nih.gov/35584… https://pubmed.ncbi.nlm.nih.gov/35050… https://pubmed.ncbi.nlm.nih.gov/28199… https://pubmed.ncbi.nlm.nih.gov/37904… https://pubmed.ncbi.nlm.nih.gov/37697… https://pubmed.ncbi.nlm.nih.gov/37217… https://pubmed.ncbi.nlm.nih.gov/34952… https://pubmed.ncbi.nlm.nih.gov/34847…
Please note that the links above are affiliate links, so we receive a small commission when you purchase a product through the links. Thank you for your support! =*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*= ~*~ Discount Coupon Code: REVERSE 🌏ProHealth Longevity 15% OFF Calcium AKG Longevity 500mg Caps https://prohealth.pxf.io/CaAKG NMN Pro™ Powder 100 g https://prohealth.pxf.io/NMN100 Longevity Greens™ Powder https://prohealth.pxf.io/LongevityGreens Full Spectrum Apigenin https://prohealth.pxf.io/apigenin Green Tea EGCG Extreme™ https://prohealth.pxf.io/EGCG 🔬Renue By Science 10% OFF Liposomal NMN caps https://bit.ly/45ChBDg Pure NMN Powder 100g https://shorturl.at/fjxU2 Lipo Quercetin 150mg https://bit.ly/3K4mwVg 🧬 DoNotAge 10% OFF Code: REVERSE https://donotage.org/?customer_referr… SIRT6 Activator® https://shorturl.at/owL23 Pure Hyaluronic Acid https://rb.gy/lcezr 🔶 Restore Our Cells Ability To Make NAD Like When We Were Young — Nuchido Time+ Supplement https://www.nuchido.com/REVERSEAGING FIRST ORDER 20% OFF Discount Code when checkout : REVERSEAGING20 🍀 iHerb New Customer 20% OFF Code: New20, existed customer 5% off All Products Link: https://iherb.co/sUBAZcqw =*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=*=
DISCLAIMER: Please note that none of the information in this video constitutes health advice or should be substituted in lieu of professional guidance. The video content is purely for informational purposes. #longevity #taurine #supplements #CaAkg #urolithinA #Nicotinamide #ALA #quercetin #EGCG #greentea #vitaminC #zinc #rutin #CD38 #Apigenin #TMG #reverseaging #supplement #slowaging #stayyoung #MethylDonors #Epigenetic #sirtuin #Exercise #NAD #BeingHungry #Rejuvenate #Mitochondria #ALA #Antioxidant #LookYounger #Resveratrol #Quercetin #Fisetin #senolytics #OliveOil #Sirtuin #HIIT #aging #Lifespan #Berberine #ReverseAging #NAD #Sirtuins #Fasting #Longevity #RestoreYouth #Healthspan #Younger #antiaging #longevity
This timelapse of future technology begins with 2 Starships, launched to resupply the International Space Station. But how far into the future do you want to go?
Tesla Bots will be sent to work on the Moon, and A.I. chat bots will guide people into dreams that they can control (lucid dreams). And what happens when humanity forms a deeper understanding of dark energy, worm holes, and black holes. What type of new technologies could this advanced knowledge develop? Could SpaceX launch 100 Artificial Intelligence Starships, spread across our Solar System and beyond into Interstellar space, working together to form a cosmic internet, creating the Encyclopedia of the Galaxy. Could Einstein’s equations lead to technologies in teleportation, and laboratory grown black holes.
Other topics covered in this sci-fi documentary video include: the building of super projects made possible by advancing fusion energy, the possibilities of brain chips, new age space technology and spacecraft such as a hover bike developed for the Moon in 2050, Mars colonization, and technology predictions based on black holes, biotechnology, and when will humanity become a Kardashev Type 1, and then Type 2 Civilization.
To see more of Venture City and to access the ‘The Future Archive Files’…
• Timelapse of Future Technology (Master List)
• Encyclopedia of the Future (Entries)
…visit my Patreon here: / venturecity.
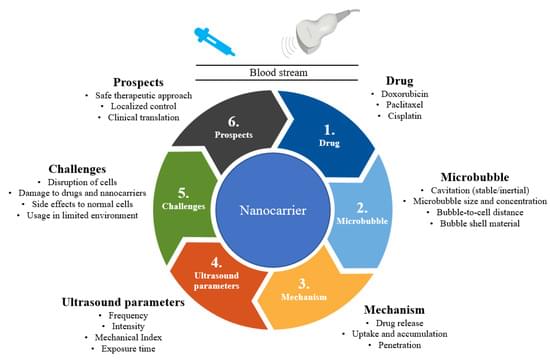
Breast cancer is the most common type of cancer and it is treated with surgical intervention, radiotherapy, chemotherapy, or a combination of these regimens. Despite chemotherapy’s ample use, it has limitations such as bioavailability, adverse side effects, high-dose requirements, low therapeutic indices, multiple drug resistance development, and non-specific targeting. Drug delivery vehicles or carriers, of which nanocarriers are prominent, have been introduced to overcome chemotherapy limitations. Nanocarriers have been preferentially used in breast cancer chemotherapy because of their role in protecting therapeutic agents from degradation, enabling efficient drug concentration in target cells or tissues, overcoming drug resistance, and their relatively small size. However, nanocarriers are affected by physiological barriers, bioavailability of transported drugs, and other factors.

A multi-university team of researchers, supported by federal funding, is developing a highly efficient bacterial therapeutic to target cancer more precisely to make treatment safer through a single $1 dose.
Traditionally, cancer therapies have been limited in their efficacy in treating patients. Some, like radiation and chemotherapy, cause harmful side effects, while others tend to result in low patient responsiveness, not to mention the cost it takes to receive treatment. Findings from the American Cancer Society Cancer Action Network recorded that 73% of cancer survivors and patients were worried about how they were going to pay the cost of their cancer care, and 51% said they were in medical debt from treatment. For example, state-of-the-art cancer therapy can cost up to $1,000,000.
Texas A&M University and the University of Missouri are leading the effort to develop a low-cost, safe, and controlled cancer treatment. Researchers received a $20 million grant from the Advanced Research Projects Agency for Health (ARPA-H) to fight cancer. The four-year project is part of the current administration’s Cancer Moonshot initiative, an effort to advance and increase funding for cancer research. It is one of the first projects funded by the newly established agency that aims to accelerate better health outcomes for everyone by supporting the development of high-impact solutions to society’s most challenging health problems.
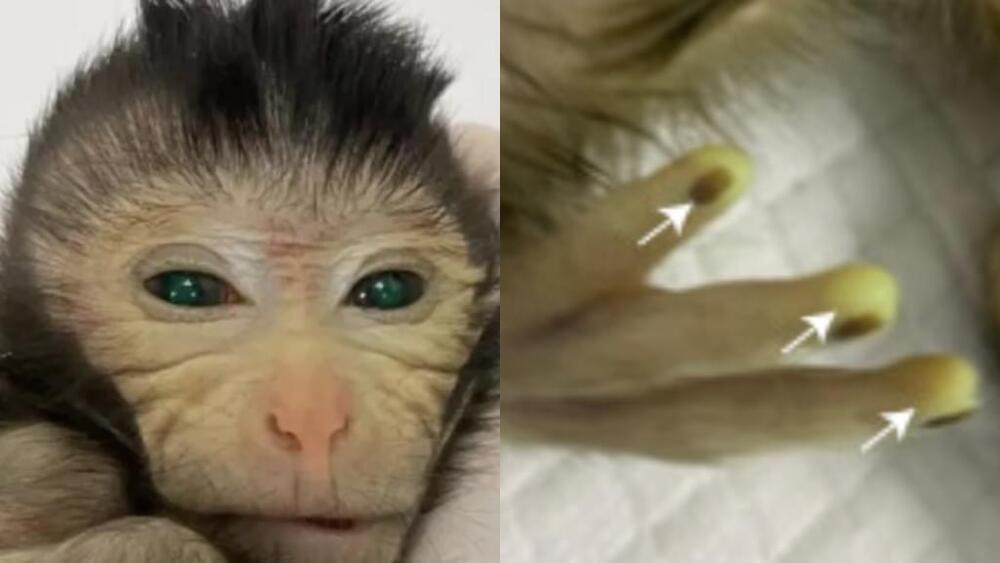
ICYMI: In a groundbreaking achievement, researchers have successfully created a chimeric monkey with two different sets of DNA through the injection of stem cells from one monkey embryo into another of the same species.
[Source]
Scientists based in China have successfully created a chimeric monkey.
How they did it: A chimera is a human or an animal whose body is composed of cells that are genetically distinct. For their study, the researchers used two sets of DNA: stem cells from a cynomolgus (crab-eating macaque) monkey and a genetically distinct four-to five-day-old embryo from the same species. After implanting embryos into 40 female macaques, they recorded 12 pregnancies and six live births.
For many people struggling with obesity, the drug is a potential lifesaver. Excess weight is associated with higher incidences of stroke, heart and liver disease, sleep apnea, joint problems, and some cancers. A major clinical trial this year in tens of thousands of overweight people without diabetes found the main ingredient in Ozempic, semaglutide, reduced the risk of stroke and heart attack, while lowering the chances of death due to cardiovascular problems.
Perhaps even more importantly, the drug is gradually changing societal views on obesity—it’s not due to lack of will power, but a chronic medical condition that can be treated.
But Ozempic and similar drugs—like Wegovy, another semaglutide-based medication that has been FDA-approved for weight loss—are already set for the next chapter: tackling a wide range of brain disorders, including Alzheimer’s and Parkinson’s. Clinical trials are underway for addiction, and the drugs are showing early promise battling bipolar disorder and depression.

Occam’s razor—the principle that when faced with competing explanations, we should choose the simplest that fits the facts—is not just a tool of science. Occam’s razor is science, insists a renowned molecular geneticist from the University of Surrey.
In a paper published in the Annals of the New York Academy of Sciences, Professor Johnjoe McFadden argues Occam’s razor—attributed to the Surrey-born Franciscan friar William of Occam (1285–1347)—is the only feature that differentiates science from superstition, pseudoscience or fake news.
Professor McFadden said, “What is science? The rise of issues such as vaccine hesitancy, climate skepticism, alternative medicine, and mysticism reveals significant levels of distrust or misunderstanding of science among the general public. The ongoing COVID inquiry also highlights how scientific ignorance extends into the heart of government. Part of the problem is that most people, even most scientists, have no clear idea of what science is actually about.”