T cells are a powerful weapon in the fight against cancer, forming the basis of treatments such as CAR-T cell therapy and checkpoint inhibitors. This research centers on another type of immunotherapy approach called T cell receptor (TCR) therapy, which engineers T cells to recognize specific proteins on cancer cells, allowing for highly targeted attacks.
Many of these proteins, however, are “self-antigens,” or molecules normally found in the body. To prevent these T cells from attacking healthy tissue, the immune system naturally eliminates the strongest cancer-fighting T cells during development. This leaves behind weaker T cell receptors that may struggle to recognize and destroy tumors, particularly those that have learned to evade immune defenses.
To overcome this challenge, researchers focused on fine-tuning naturally occurring T cell receptors to strengthen their ability to recognize a common prostate cancer protein called prostatic acid phosphatase (PAP), which is commonly expressed on prostate tissue and prostate tumors. The team identified a naturally weak TCR, known as TCR156, that could detect PAP but was not strong enough to effectively kill cancer cells.
Using a novel technique called catch bond engineering, a concept developed by the Lab, the researchers “turbocharged” the T cells. In the body, T cells form brief, mechanical bonds with their targets, known as catch bonds, which help them sense and respond to threats. By altering just one or two amino acids in the T cell receptor, the scientists were able to strengthen these bonds while preserving the T cells’ natural ability to recognize their specific target.
Multiple engineered versions of TCR156 were created and tested. Two candidates proved to be the most effective. These engineered T cells were analyzed for their ability to recognize tumors, release cancer-killing molecules, proliferate, and resist exhaustion. Advanced imaging, single-cell RNA sequencing, and structural analyses were used to confirm that the modifications improved T cell function while maintaining precision and avoiding off-target effects.
Structural and computer modeling studies showed that the catch bond mutations did not change the overall TCR shape but primed it to form a new interaction with PAP when the T cell engaged the tumor, explaining how the engineered T cells could remain highly specific while dramatically boosting their cancer-killing ability.
The researchers found that a single amino acid change created a catch bond hotspot that significantly enhanced T cell function. This change did not directly contact the cancer protein until the T cell engaged dynamically, demonstrating that a tiny modification can have a major effect. Most importantly, the modifications did not make the cells attack healthy tissue.
The strength and lifetime of the TCR’s bond with PAP under force were better predictors of tumor-killing ability than traditional measures of binding strength. In laboratory experiments, the engineered T cells showed longer contact with cancer cells, greater secretion of tumor-killing molecules such as Granzyme B, IFNγ, and TNFα, and improved proliferation while resisting exhaustion.
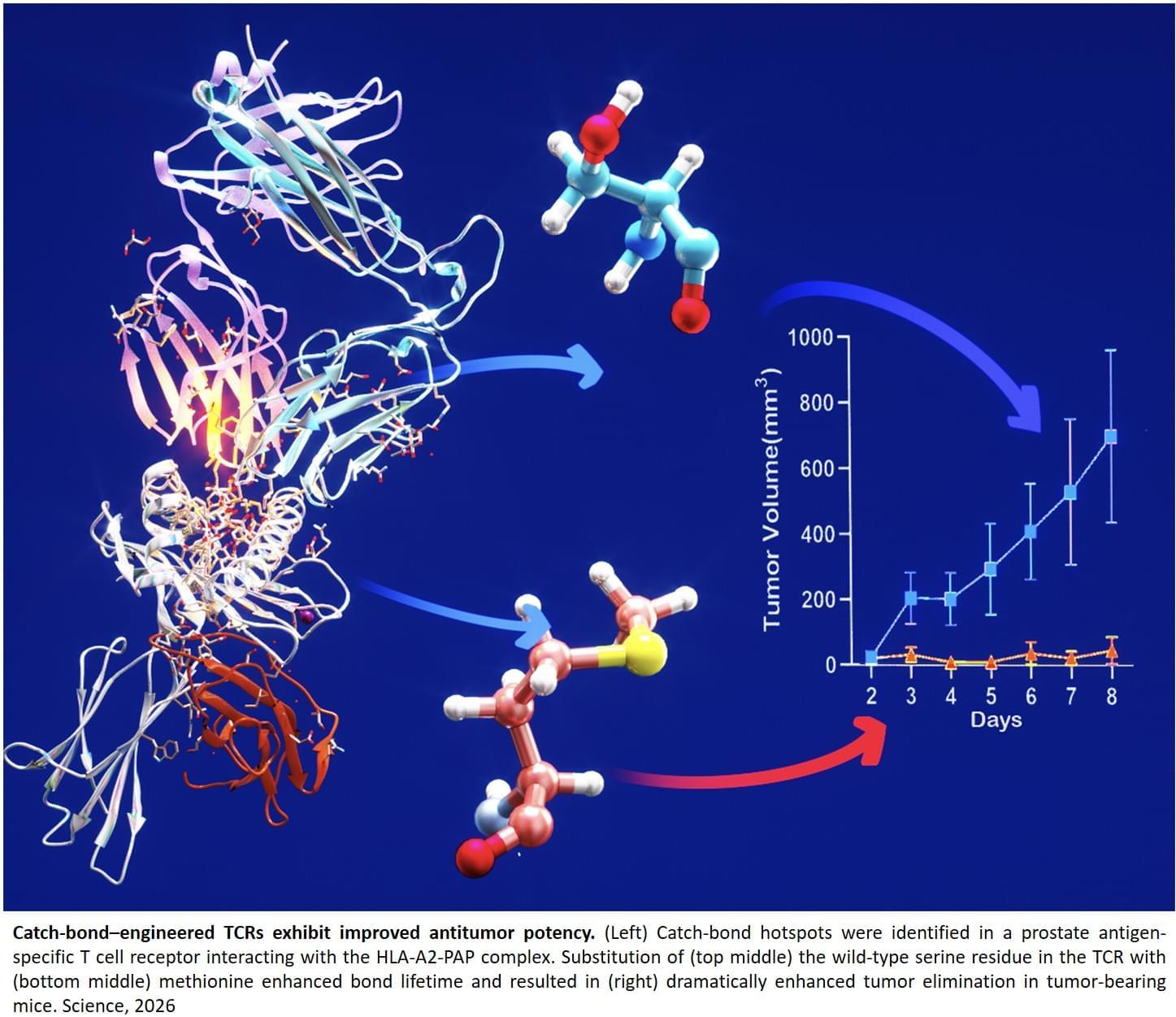
In mouse models, the engineered T cells had delayed or completely halted tumor growth, while those receiving unmodified T cells showed little effect. Analyses of the immune cells inside the tumors revealed that the engineered T cells were better able to persist, maintain a stem-like state, and resist exhaustion, a common limitation of immune therapies. ScienceMission sciencenewshighlights.
The researchers have engineered a new class of supercharged T cells that are stronger, longer-lasting, and more precise at killing prostate cancer cells by fine-tuning how they physically interact with tumor cells.
Instead of simply making T cell receptors bind more tightly to cancer, the team introduced a natural “catch bond,” a fishhook-like interaction that strengthens when cells pull against each other. This allows T cells to latch onto cancer cells more effectively at the moment they attack, helping them recognize the tumor, stay engaged longer and deliver a more powerful and targeted immune response without damaging healthy tissue.
The approach, described in the journal Science, represents an important step toward developing safer, more effective T cell therapies for prostate cancer and could potentially be adapted to treat a wide range of other tumors.