Immunotherapy resistance remains a significant clinical challenge in the treatment of colorectal cancer. A recent study by Mount Sinai researchers, published in Cell Reports Medicine, reveals that overcoming this resistance requires more than just activating cancer-fighting T cells; it depends on restoring crucial communication between T cells and myeloid cells, specifically macrophages. Using advanced preclinical models and single-cell analyses, the research team identified exhausted T cells and immunosuppressive macrophages as key drivers of treatment failure. To counter this, they tested a novel combination therapy that targets multiple immune checkpoint proteins (PD-1, CTLA-4, and LAG3) alongside TREM2, a marker found on suppressive macrophages. By successfully reprogramming the tumor microenvironment to simultaneously reinvigorate T cells and neutralize suppressive macrophages, this combination strategy achieved up to 100% tumor clearance in mismatch repair-deficient cancer models and over 70% clearance in typically resistant mismatch repair-proficient models. Furthermore, the approach established long-lasting immune memory against cancer recurrence, highlighting the profound clinical potential of rationally designed combination immunotherapies that address both T cell dysfunction and the suppressive tumor environment.
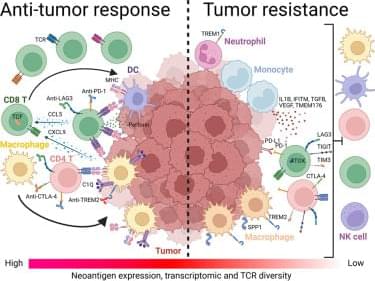
Mestrallet et al. show that T cell-myeloid interactions determine response to PD-1 blockade in colorectal cancer. Targeting TREM2 macrophages together with LAG3, CTLA4, and PD-1 reprograms the tumor microenvironment and drives antitumor immunity, achieving up to 100% tumor clearance in mismatch repair-deficient and 70% in mismatch repair-proficient models.